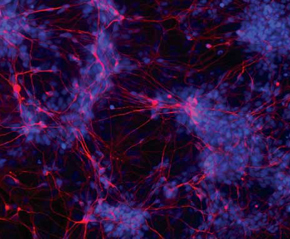
KARINA GRIESI OLIVEIRAAutist’s neurons: morphology changesKARINA GRIESI OLIVEIRA
One of the most common neurological disturbances in newborns, autism is a disease whose origin is complex and that has challenged medical research for decades. It is likely that environmental factors, such as exposure to heavy metals, pesticides or other toxic agents may play a part in the appearance of this troubling condition or in the increase of its symptoms. However, most of the studies are trying to make progress in terms of understanding autism’s intricate genetic basis, as it might be caused by an as of yet unknown number of mutations and alterations in different genes of segments of the human genome. A team of Brazilian researchers believes that they have found a clue to one of the mechanisms that might underlie the manifestation of this disease, characterized by repetitive behaviors and serious communication and social integration difficulties.
Using the baby teeth of a five-year old autistic child seen to at the Center of Human Genome Studies at the University of São Paulo (USP), one the Cepids (Centers for Research, Innovation and Dissemination) financed by FAPESP, the scientists obtained induced pluripotent stem cells (iPSC) and transformed them into neurons in their laboratory. Thus, they managed to observe an important alteration in a given calcium channel whose sound functioning is extremely important in the early stages of the neuron development process. “There is less calcium altering the activation of cell pathways that might be connected to the appearance of autism, in this case,” geneticist Maria Rita Passos Bueno, from USP, comments, one of the authors of the as yet unpublished study. She has been analyzing the genetics of autism for a decade. The obtaining of a lineage of iPSC and of neurons with autism took place at the laboratory of a Brazilian scientist, Alysson Muotri, at the University of California in San Diego (UCSD), where one of Maria Rita’s PhD students, the biologist Karina Griesi Oliveira, spent one year learning this new cell reprogramming technique. The neurons of autists also have different morphology than that of normal nervous cells, according to scientific literature. They have a smaller nucleus and a smaller number of ramifications. “This might mean that there is a problem of development or of maturing of the neurons,” states Muotri.
The hypothesis seems to make sense, given that the Brazilian’s team in San Diego achieved similar results when they studied the neurons of patients with Rett syndrome, another brain development disorder. These neurons were also obtained from iPSC cells, derived from skin. Although this condition has some symptoms that are similar to classic autism, it affects almost only girls and has a fairly precise cause: mutations in the MeCP2 gene of the X chromosome cause most of the cases of this disease. This gene contains the instructions for the synthesis of a protein, also called MeCP2, that is important for brain development and that works like a biochemical key for regulating other genes. Anomalies affecting the production of this protein change the way in which other genes behave. Coincidentally, in the case of the neurons derived from the iPSC of the Rett syndrome patients, the researchers found alterations in chemical pathways that also depend on calcium for their activation, a dysfunction similar to the one found in the Brazilian autistic patient. “Perhaps the MeCP2 protein is important to regulate the calcium pathway,” says Muotri.

KARINA GRIESI OLIVEIRAiPSC cellsKARINA GRIESI OLIVEIRA
Chromosome rearrangement
At the current stage of these studies, it is impossible to say whether the calcium channel is involved in all cases of autism (and of other similar neurological disorders) or only in a small number of manifestations of the disease. Concerning Rett’s syndrome specifically, the situation is simpler. This disease’s genetic cause is known and animal models indicate that, if the levels of MeCP2 are normalized, the syndrome’s symptoms diminish. When it comes to autism, however, the situation is more complex and nuanced. There is no single gene or group of genes linked to the manifestation of the disease. Certain genetic alterations connected with autism are known, but it is unknown how many more might exist. The Brazilian child that supplied the baby teeth for the USP and UCSD teams to work on, for instance, developed autism because of a rare alteration involving segments of two chromosomes. A stretch of the genetic sequence normally found in chromosome 3 changed places with a piece of chromosome 11. These so-called karyotype rearrangements of the set of chromosomes in an organism can cause diseases. Still, “fewer than 5% of autistic people have chromosome rearrangements,” says Karina.
At the Center of Human Genome Studies, the researchers characterized two other cases of autism due to this kind of genetic abnormality, one with a rearrangement of chromosomes X and 2 and another with changes in chromosomes 2 and 22. With the help of the researcher Matthew State from Yale University, Karina was able to precisely identify the point where the chromosomes of the three patients studied had a break. Sometimes, this occurs in the middle of the sequence of a gene, which, once damaged, stops functioning. If it is an important gene, this can cause problems. “If we find more mutations or genetic rearrangements linked to autism and to problems in the activation of this calcium channel, then the hypothesis that this chemical pathway really is important for the disease to appear will become stronger,” says Maria Rita. If this idea proves to be correct, the researchers may, in the future, investigate the effect of pharmaceutical products that act upon this chemical pathway in animal models with a condition similar to autism, or directly with human neurons, derived from iPSC cells. “We can try to develop new compounds or even to test known molecules that are currently available in the inventory of drugs in biotechnology companies. Using neurons derived from the iPSC of each patient for new drug trials is the first step toward personalized medical treatment,” states Muotri.
Republish