
CDC
Illustration showing skin lesion caused by the bacterium that causes Hansen’s disease (red rods)CDCMore than 25,000 new cases of Hansen’s disease each year position Brazil in second place globally, behind only India in the ranking of the countries with the highest rate of growth of this disease, and also one of the most affected. Nevertheless, Brazil is close to reaching the goal set by the World Health Organization (1 case per 10,000 inhabitants) for Hansen’s disease to no longer be considered a public health problem. The detection rate is 1.22 cases per 10,000 and appears to be declining: between 2007 and 2016, the number of new cases of Hansen’s disease fell 37% in Brazil, according to the Brazilian Ministry of Health.
These data would be encouraging if not for one detail: behind these numbers there may be many undiagnosed patients. This was indicated in a study published in February of this year in the journal PLOS Neglected Tropical Diseases. The study was performed by researchers at the Alfredo da Matta Foundation for Tropical Dermatology and Venereology (FUAM), an agency linked to the Amazonas State Department of Health, in collaboration with Amazonas State University and other institutions. The results of this study suggest that in Manaus, the incidence of Hansen’s disease in children and adolescents under age 15 is 17 times higher than the rate recorded previously for this age group in the city. In 2013, the rate in the capital of Amazonas was 0.68 cases per 10,000 people, but the FUAM study showed an occurrence of 11.58 cases per 10,000, indicating underreporting of the disease.
The study was conducted in 277 of the 622 public schools in Manaus. Forty new cases of the disease were found among the 34,547 students examined. According to dermatologist Carolina Talhari, the study coordinator, this number is especially concerning because of the patient age group. “From an epidemiological point of view, the existence of children with Hansen’s disease signals the presence of the bacteria circulating in the community,” she warns.
Altemar Alcantara / SEMCOM
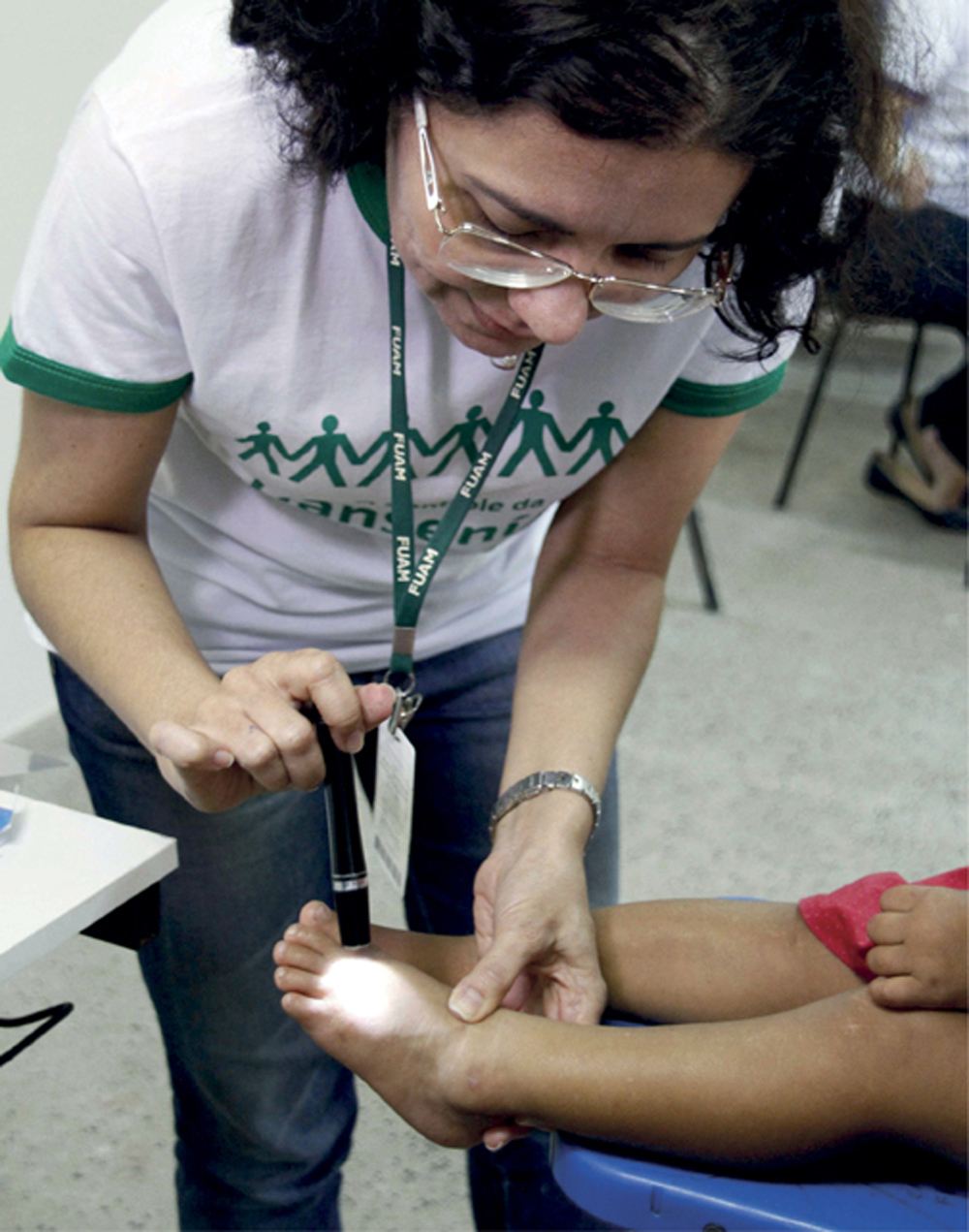
Child undergoes dermatological examination in Manaus in January of this yearAltemar Alcantara / SEMCOMHansen’s disease affects all ages, but occurrence in children and adolescents under 15 years of age is an important epidemiological marker for the disease, explains the researcher. The disease (known in the past as leprosy) is caused by the bacterium Mycobacterium leprae, which is transmitted from person to person through contact with secretions released when untreated infected people cough or sneeze. The disease affects the peripheral nerves and causes whitish or reddish spots on the skin which lose sensitivity. The incubation time is long, from five to 10 years before the onset of symptoms, which makes it difficult to ascertain how much time has passed since exposure to the bacteria when an infected adult is found. Meanwhile, detection in children indicates the existence of active foci of transmission, generally in the home environment.
A disease of agglomeration
The Manaus study found that 52.5% of the cases of recently diagnosed children had contact with at least one infected person at home. Grandparents were the transmitters in 52.4% of the cases, aunts or uncles in 14.3%, and parents in 9.5%. “Infection of the child occurred before the adult began treatment, since we know that the first supervised dose of multi-drug therapy fragments the bacilli, interrupting transmission,” says epidemiologist Valderiza Pedrosa, a researcher at FUAM and lead author of the article in PLOS Neglected Tropical Diseases. The treatment, which is available for free through the public health network, involves administration of three drugs (sulphone, rifampicin, and clofazimine). The regimen is effective and has few side effects, but takes 9 to 18 months.
The researchers also examined 196 people who lived with the infected children, in the home environment or in neighboring houses. They maintain that it is important to evaluate unrelated people who live near the infected cases, since a survey conducted five years ago indicated that the detection rate was similar among family members as well as neighbors.
This study, which was published in 2013 in PLOS Neglected Tropical Diseases, was conducted by the Department of Tropical Medicine at the Federal University of Rio Grande do Norte in the city of Mossoró, which is considered hyperendemic for leprosy. Professor Selma Maria Bezerra Jerônimo, the director of the department, explains how the infectious agent is transmitted between neighbors: “The bacillus is suspended in the air and survives for a few days in the environment. It so happens that in many locations the houses are combined, sharing a partial wall and a common roof above without a ceiling under it. People share the same contaminated air.”
Detection of the disease in children indicates the existence of active foci of transmission
Besides continuous exposure to the bacillus, there are also genetic factors involved in the epidemiology of Hansen’s disease. Although coexistence with an infected, untreated person is the greatest risk factor for infection, the majority of exposed persons do not develop the disease. However, the FUAM research group found a family in which the disease affected three generations.
The geneticist Marcelo Távora Mira, a professor in the Graduate Program in Health Sciences at the Pontifical Catholic University of Paraná, explains that the genetic component defines a person’s susceptibility to contracting the disease. “It is unlikely that there is a ‘Hansen’s disease gene’. Today the research indicates a genetic effect caused not by one or a few genes, but rather a dozen genes, each partially contributing to the overall observed effect,” says Mira. “However, we are still far from the point when a genetic test can be applied to identify susceptible individuals.” According to the geneticist, early diagnosis is still essential in fighting Hansen’s disease, and this depends on training doctors and support teams in the public health services.
Conflicting data
According to a note from the press department at the Ministry of Health, preliminary data from 2017 indicate an incidence of 0.6 cases of Hansen’s disease per 10,000 inhabitants in Manaus; in other words, 127 new cases were diagnosed, four in children under 15 years of age. The agency stated that the official results of the prevalence of this disease in Brazil include patients of all ages. As a result, it maintains that the results published in the PLOS Neglected Tropical Diseases article, which looked at children and adolescents aged under 15, cannot be compared with the official data. Carolina Talhari disagrees. “The detection rate found for Hansen’s disease in children in our study was compared with the official rate of detection for the same age range,” she says. “It is necessary to invest in an active search and in the early detection of cases.”
 For Marco Andrey Cipriani Frade, a professor of the University of São Paulo Medical School in Ribeirão Preto (FMRP-USP) and vice president of the Brazilian Society of Hansenology, the numbers from the Manaus study do not represent isolated cases. They confirm a worrying scenario which has been described in several studies. “We have been harping on this same thing since 2012,” says Frade.
For Marco Andrey Cipriani Frade, a professor of the University of São Paulo Medical School in Ribeirão Preto (FMRP-USP) and vice president of the Brazilian Society of Hansenology, the numbers from the Manaus study do not represent isolated cases. They confirm a worrying scenario which has been described in several studies. “We have been harping on this same thing since 2012,” says Frade.
He also participated in studies in various places where undiagnosed cases of Hansen’s disease were recorded in children. In the cities of Oriximiná and Castanhal, both in Pará, 109 new cases were detected among 754 individuals examined (an incidence of 14.4%), 40 in children younger than 15. The study was published in 2015 in the journal BMC Infectious Diseases. Pará is among the Brazilian states which are most affected, alongside Maranhão, Piauí, Rondônia, Roraima, and Pernambuco. The incidence is even higher in Tocantins and Mato Grosso, where the disease is considered hyperendemic.
The Manaus study confirms a worrying scenario, says Marco Frade of the Brazilian Society of Hansenology
The researchers at FMRP-USP did not limit their focus to only the states with the highest incidence of Hansen’s disease; in the municipality of Jardinópolis, approximately 20 kilometers from Ribeirão Preto in the interior of São Paulo, 24 new cases of the disease were found between July and December 2015. In addition to measuring the incidence (number of new cases), they also verified the prevalence (total number of cases). “In 2014, the prevalence of Hansen’s disease in Jardinópolis was 0.73 cases for each group of 10,000 inhabitants. In 2015 and 2016, with the intensification of the active search for cases by the staff at the National Reference Center for Sanitary Dermatology at the Hospital das Clínicas in Ribeirão Preto, the rates rose to 4.4 and 23.6, respectively,” explains Frade.
He adds that health professionals have difficulty diagnosing the disease because of a lack of preparation and because there is the mistaken notion that Hansen’s disease is ceasing to be a public health problem in the country. “Those who look and know what they are looking for find the disease,” he says.
Scientific articles
PEDROSA, V. L. et al. Leprosy among schoolchildren in the Amazon region: A cross-sectional study of active search and possible source of infection by contact tracing. PLOS Neglected Tropical Diseases. Feb. 26, 2018.
MOURA, M. L. et al. Active surveillance of Hansen’s Disease (leprosy): Importance for case finding among extra-domiciliary contacts. PLOS Neglected Tropical Diseases. Mar. 14, 2013.
BARRETO, J. G. et al. Spatial epidemiology and serologic cohorts increase the early detection of leprosy. BMC Infectious Diseases. Nov. 16, 2015.