
LÉO RAMOS
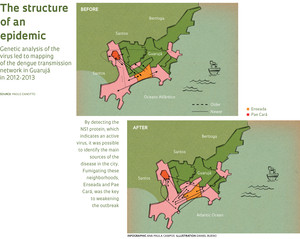
Aedes aegypti larvae developing in the laboratory to form a transgenic lineLÉO RAMOSIt was not the beach that attracted Paolo Zanotto and Julian Villabona-Arenas to the city of Guarujá along the southern coast of São Paulo State in the summer 2012-2013. Zanotto, a virologist at the Institute of Biomedical Sciences of the University of São Paulo (ICB-USP), and Villabona-Arenas, a PhD student, were monitoring cases of dengue and analyzing the genetics of the virus to reconstruct a grid of how it spreads throughout the population. Guarujá was selected for its proximity to the São Paulo metropolitan area. Their analysis showed that two neighborhoods, Pae Cará and Enseada, were the disease’s main focal points, from which it then moved to other parts of the city. The work of the researchers caught the attention of an employee of the local health surveillance department, who realized the value of knowing where the cases with active virus were, and she summoned a fumigation unit—the so-called “fogging”—to kill the mosquitoes in these locations. “They went right to the head of the dragon and shot it,” says Zanotto. Thereafter, the maps showed a situation that was much easier to control, with only a few cases. “That’s what needs to be done in every city,” he says, while also noting the need to combine it with vaccines and other forms of control to combat the mosquito that transmits the disease.
The work of Zanotto’s group has been pointing out ways to combat dengue and underscoring the increased risk of epidemics. One reason for the alarm is the presence of the four serotypes of the virus they observed in Guarujá that summer, as shown in a 2014 article in PLOS Neglected Tropical Diseases. Its proximity to the port of Santos, where mosquitoes and viruses can disembark as stowaway passengers, most likely has an impact. In Jundiaí, which is very close to the São Paulo Metropolitan Region, the researchers found only serotypes 1 and 4, but this is hardly a relief. Together, the two municipalities have shown that the São Paulo state capital is subject to multiple viruses, creating a situation known as hyperendemicity, which increases the risk of a person being infected several times and raises the risk of hemorrhagic-type cases. “The presence of the four serotypes in an outbreak in one of Brazil’s most densely populated areas is a disturbing finding,” says Villabona-Arenas. “For many years this co-circulation had been documented only in countries of southwest Asia and more recently in India; it is always associated with greater disease severity among children.”
Indeed, the latest figures offer no reason to relax, although the immediate fear of the Aedes aegypti mosquito, which transmits the disease, begins to recede with the arrival of cold and drought, which do not favor larval development. The Southeast region was the stage for 66% of the almost 746,000 cases recorded by the Ministry of Health in all of Brazil from early 2015 to April 18, 2015. The number of cases is less than that recorded in 2013, but much more than in 2014. This total represents different degrees of severity—some people barely feel any symptoms, while others experience high and persistent fever and spend long days prostrate with intense body aches and nausea, which makes it impossible to follow the prescription to drink plenty of fluids. During this period, there was confirmation of 414 serious cases and 5,771 cases with warning signs, categories that require medical attention. This was far more than the previous year, with a high proportion in the state of São Paulo. Severity factors of the disease include liver damage and an alarming drop in the concentration of platelets in the blood, which can transform microscopic lesions into a hemorrhage.
Zanotto believes the numbers and the occurrence of hyperendemicity indicate an alarming progression of the disease. “Dengue fever is just beginning in Brazil,” he says, based on a chart of the number of cases since 1995, which predicts a sharp escalation from now on. It means, in his opinion, that efforts to combat epidemics of the disease have to become more effective. “We should emulate the fire department, which acts on small fires, aiming to contain them before they spread and get out of control.”
 Zanotto’s studies in cities like Guarujá, Jundiaí and São José do Rio Preto are finding dengue outbreaks in areas that have the lowest socioeconomic indicators. But concentrating efforts in the slums is not enough, according to a study done by biologist Ricardo Vieira Araujo, today a specialist with the Global Climate Change Coordination unit of the Ministry of Science, Technology and Innovation (MCTI), and published in 2015 in the Brazilian Journal of Infectious Diseases. He showed that parts of the city of São Paulo with a significantly higher surface soil temperature, low humidity, little vegetation coverage, and low levels of soil permeability—heat islands—have a higher incidence of dengue.
Zanotto’s studies in cities like Guarujá, Jundiaí and São José do Rio Preto are finding dengue outbreaks in areas that have the lowest socioeconomic indicators. But concentrating efforts in the slums is not enough, according to a study done by biologist Ricardo Vieira Araujo, today a specialist with the Global Climate Change Coordination unit of the Ministry of Science, Technology and Innovation (MCTI), and published in 2015 in the Brazilian Journal of Infectious Diseases. He showed that parts of the city of São Paulo with a significantly higher surface soil temperature, low humidity, little vegetation coverage, and low levels of soil permeability—heat islands—have a higher incidence of dengue.
From 2009 to 2013, Araujo worked at the Health Surveillance Coordination unit of São Paulo, monitoring vector-borne and zoonotic diseases in the city. “I wondered why a slum in the south recorded so many cases, while in another community in the north, for example, with similar characteristics, the numbers were much lower,” he says. In the same period, the city’s Department of the Environment concluded a mapping of the surface soil temperature, which pointed toward heat islands in the capital. “But many researchers thought the islands themselves would be in regions with the lowest socio-economic indicators, and a higher population density. So perhaps the cause was not related to temperature, but instead to the social and demographic conditions.”
In order to distinguish among the factors, more than one set of data was needed. The 2010 census by the Brazilian Institute of Geography and Statistics (IBGE) made it possible to calculate population, population density, average income and the predominant form of urban occupancy in the 96 administrative districts of São Paulo. The data also indicated where there were favelas, occupancies and tenements. By using satellite imagery, it was possible to analyze the vegetation cover, as well as create a map with the average surface temperatures of the entire city. Records of indigenous dengue cases came from the Health Surveillance Coordination unit, which recorded about 7,400 cases from 2010 to 2011.
Combining the information showed that 93% of the cases occurred where the average surface temperature was more than 28 degrees Celsius. In areas with greater vegetation coverage the number of cases per 100,000 inhabitants was only 3.2, versus 72.3 cases in less wooded areas. In all, the type of occupancy seems to have less of an influence on the incidence of dengue than the temperature during the analyzed period.

LÉO RAMOS
The green glow on the head and tail of the larvae is the marker indicating genetically modified insectsLÉO RAMOSThe study went more in depth to also include a laboratory experiment with two lines of Aedes aegypti: one line routinely used by researchers and another obtained from eggs collected on the campus of USP. The influence of temperature became quite clear: when it reaches 32°C, more than 90% of the insect larvae become adults.
Araujo cautions that the maps of heat islands are not static, and the data would require frequent updating. Still, he believes it is important for health and urban infrastructure professionals to act together in an integrated manner. “Increasing the number of green areas is one approach. But it is worth remembering other alternatives, such as those adopted in villages along the Mediterranean coast, where houses are painted white as a way to lessen the heat. We need to use the resources we have to fight dengue in a strategic and integrated manner,” he says.
Winged virus
One of the existing resources in the fight against mosquitoes is the use of insecticides, as was the case in Guarujá. The problem is that, because insecticides are the most often used strategy, Aedes aegypti has developed a resistance to the most common ones, which are based on pyrethroids; they are undeterred by most repellents and will continue to hang around, with their nervous flight, feasting on their victims. While pursing her doctorate at São Paulo State University (Unesp) in Botucatu, biologist Maria de Lourdes Macoris monitored a number of mosquito populations in São Paulo State and found that their resistance remained intact even after 15 years without pyrethroids. “The use of insecticides targeted resistant populations,” says biologist Paulo Ribolla, advisor to Macoris. “Some municipalities are already using other products, with greater success.” In his laboratory, he is now implementing technology to produce mutant mosquitoes and investigate which genes are responsible for the resistance.
In the evolutionary race with mosquitoes, it is necessary to seek new insecticides that are effective and act comprehensively where they breed. Since 2007, this has been the goal of the research group coordinated by Eduardo José de Arruda, a chemical engineer at the Federal University of Grande Dourados (UFGD) in the central-western state of Mato Grosso do Sul. “We conducted a survey of the Aedes aegypti and the Culex quinquefasciatus mosquitoes, and we found that the insects were already resistant to some classes of insecticide,” says Arruda. “We could kill all the adults of a generation, but the eggs left in the breeding areas, despite the loss of viability, could still hatch and replenish the population in a matter of months.”

LÉO RAMOS
Once aligned…LÉO RAMOS“Classes of insecticides to which resistance has developed should no longer be used to control the mosquitoes,” says Arruda, who underscores the economic and environmental costs of the increased amount of insecticides required. The group he coordinates, along with partners from other universities, is looking to synthesize and classify multifunctional compounds that prevent the eggs from hatching and kill the larvae. They also destroy the bacteria, fungi and protozoa that constitute the mosquito diet, and can interfere with the chemical communication that attracts the females to the breeding areas where they deposit their eggs. The idea is to find strategies to control two or three insect generations at the same time and break their reproductive cycles.
Because they are more comprehensive the multifunctional compounds require special care. For a Master’s degree at UFGD, Taline Catelan examined the effects of four phenolic insecticides on the eggs of Aedes aegypti and Artemia salina, a small crustacean that lives in the water. “Artemia salina serves as an indicator of potential damage to water sources,” says Arruda. The study, published in 2015 in Advances in Infectious Diseases, showed that one of the compounds completely prevented the hatching of the mosquito eggs, but also affected the Artemia populations.
More promising still are the results of studies with metal-insecticides, which contain copper or iron. The compounds unleash an oxidative stress reaction that can cause lethal damage to cells and tissues. “It’s as if we used a Trojan horse to carry the compound inside the cells, and the active metabolism of the insect produces the pesticide in situ,” says Arruda.
Sleeping with the enemy
Given the uncertainty surrounding the effectiveness of insecticides, other weapons need to be found. Margareth Capurro is a biochemist whose laboratory at ICB-USP focuses directly on small insects with striped legs, in an unusual way: by producing thousands and thousands of them to release into the environment. “I have become a global consultant on the mass production of mosquitoes,” she says, and during the preparation of this report, she traveled to China to do just that. At a factory located in Juazeiro, in the state of Bahia, Capurro worked with Moscamed Brasil to implement production of a line developed by the British company, Oxford Insect Technologies (Oxitec). These genetically altered mosquitoes accumulate a protein that makes the larval cells collapse, and the larvae never reach adulthood (see Pesquisa FAPESP Issue No. 180). Last year, her team published a video in the Journal of Visualized Experiments showing the production process, including the laborious task of separating male and female pupae by size (females are larger).

LÉO RAMOS
…the eggs receive injections that induce genetic modificationsLÉO RAMOSThis separation is necessary because only males, which neither bite nor carry the virus, are released into the wild to mate with wild females, which then produce modified and unviable offspring. To achieve this production, all the infrastructure and logistics were provided by Moscamed. The company also signed partnership agreements with the Ministry of Health and the Bahia State Health Department, which have helped fund the initiative. At first, the team had to enlist reporters to assist in communicating with the local population. “We could not arrive in the city and just start releasing mosquitoes,” says Capurro. “We went into people’s homes to talk to them and explain the project; we used radio, television, and local media.”
But just because this production exists does not mean the research ends. The Oxitec mosquitoes continue to be tested in the laboratory to see how the dengue virus behaves in the host. With this knowledge, we have to always return to the field, in a continuing process. “In a small pot everything works, but in the environment, does the altered mosquito fly as much as the wild one?” Capurro asks. She already knows that it can fly. Another problem is to produce males compatible with the female population of the Bahian scrublands. In the laboratory they grow too much, like any animal fed as much as it wants to eat and gets no exercise. It was necessary to find the right number of larvae to be developed in a given volume of water, and the right amount food to give them.
Tests in Juazeiro, up to 2013, and in Jacobina, both in Bahia State, which began that same year, have shown that the system works, despite some setbacks. “The mating frequency is lower, so we have to increase the number of mosquitoes.” The release has to be constant, but with weekly adjustments to the insect population. With the transgenics, the number of them decreased in every city. But Capurro cautions that efforts to search for breeding areas have to be maintained.
The partnership with health officials indicated the need to improve procedures. “They found breeding areas with larvae and had no way of knowing whether or not they were viable,” says Capurro. The solution was to invest in developing sterile males in the laboratory. As the female mates just once in her lifetime and stores seminal fluid, a single mating with a sterile male is enough for her to be unable to produce offspring. But this transgenic line is not yet where it needs to be, with a sterility rate of between 30% and 40%. Controlled mating takes more time to get to the final product, according to Capurro.
 Another genetic manipulation under development aims to prevent the birth of females, a process called sex reversal that produces an entirely male line. This would increase the factory’s productivity, since right now 50% of the larvae are female, and some larvae are lost during the pupae separation process. “We lose between 15% and 25% of the males,” says Capurro. If the double, sterile and sex reversal transgenics work, it is not just the productivity that will improve. Right now the male larvae need to be shipped in refrigerated cars to Jacobina. If indeed only males are to be produced, then the larvae can be sent by mail on sheets of paper with the eggs attached.
Another genetic manipulation under development aims to prevent the birth of females, a process called sex reversal that produces an entirely male line. This would increase the factory’s productivity, since right now 50% of the larvae are female, and some larvae are lost during the pupae separation process. “We lose between 15% and 25% of the males,” says Capurro. If the double, sterile and sex reversal transgenics work, it is not just the productivity that will improve. Right now the male larvae need to be shipped in refrigerated cars to Jacobina. If indeed only males are to be produced, then the larvae can be sent by mail on sheets of paper with the eggs attached.
The results are promising, but may not be enough. “If we eliminate mosquitoes, dengue ends; if we only reduce the population, the disease may strike again after a few years,” explains Capurro. This is what happened in Singapore in the early 2000s. With a reduced number of mosquitoes, the proportion of infected insects increases. As human resistance also drops without exposure to the virus, the risk is of a strong resurgence and an epidemic.
So Capurro and PhD student, Danilo Carvalho, are proposing to fight mosquitoes in two phases, as explained in a 2014 article in Acta Tropica. It would work like this: after reducing the population by using sterile males, a second line would be released, currently under study in the laboratory; it would carry a mutation allowing the mosquito to recognize the cells of its own digestive system; the virus inside the cells would replicate and destroy those very cells.
Internal Battle
No matter how much one fights mosquitoes, the disease will not be easily eradicated and requires the help of the immune system. A vaccine has been touted as imminent, but it is unlikely to be available immediately. The most imminent is the one produced by the French laboratory Sanofi Pasteur, which is awaiting approval by the Brazilian Health Surveillance Agency (Anvisa) and is expected to enter the Brazilian market in 2016. But Luís Carlos de Souza Ferreira, a microbiologist ICB-USP, remains unconvinced of its efficacy. He says that this vaccine is based on the yellow fever virus. Only part of the genome responsible for the structural proteins belong to the dengue virus.
“It was believed that this was enough, because antibodies recognize an invader on the basis of these proteins,” he says. But his group and others have shown that, in the case of dengue, when levels of these antibodies are low or they are less efficient, the remaining viruses are carried to the cells where they replicate. Destroying these cells is the task of the T lymphocytes, and their main target is other proteins of the virus—the non-structural ones. “Our research has shown that the T-lymphocyte response is important in dengue,” he says. According to Ferreira, this does not occur in the vaccine produced by Sanofi Pasteur.
One of Ferreira’s lines of research is indeed to produce a vaccine based on one of these proteins, the NS1. Famous for being the marker indicating that a person suffering from body aches is infected with the dengue virus, the protein has been shown to be a good target, as reported in a 2014 review article in Virus Research. “We produce the NS1 in bacteria and purify it for use as a vaccine component,” says Jaime Henrique Amorim, a postdoctoral researcher and lead author of the article. “We achieved 50% protection in tests on mice; it is a promising formulation, although still far from becoming a product for use in humans.”
Aside from this more applied aspect, the studies conducted in the laboratory have another dimension: to understand the immune response pattern. This focus can assess and guide the development of other vaccines, and has led Ferreira and Amorim to believe that the vaccine now in clinical trials at the Butantan Institute is the most promising. “Studies carried out in the United States have shown that this vaccine, based on weakened forms of the four types of dengue virus, provokes a response similar to that of people who have been infected and were able to neutralize the virus,” says Amorim.
Produced in Brazil, the vaccine was developed in the United States at the National Institutes of Health (NIH). “We are currently finalizing the Phase 2 clinical trial,” says Dr. Alexander Precioso, director of the Special Laboratory for Clinical Trials and Pharmacovigilance at the Butantan Institute. He hopes to have all results collected, analyzed and released by late June 2015.
According to Dr. Precioso, 300 people have been tested, which shows that the vaccine is safe. These results led the Institute to ask ANVISA for authorization to commence Phase 3, even before all the data had been collected from Phase 2. “We need to start as soon as possible to recruit volunteers to get vaccinated before the next dengue season begins,” says Dr. Precioso. If all goes well, volunteers could be vaccinated as soon as Phase 2 is complete. This schedule would allow the immune response to the vaccine to be tested next summer, the season when dengue outbreaks occur in several regions of Brazil. It depends on being able to recruit volunteers, which should number at least 17,000 people from across the country, on the characteristics of the next outbreak, and how those who are immunized respond. The Butantan plan includes registration of the vaccine as soon as efficacy data have been demonstrated, and monitoring participants for at least five years, to assess the durability of the immune response and determine the need and frequency of vaccine boosters.
There seems to be a consensus: there is no single solution, in terms of strategy or geography. In cities like Rio de Janeiro and São Paulo, the highest incidence occurs in summer, when there is more rain and the temperature is high. Yet in the Northeast it is the drought that causes the disease to affect more people, when long periods without rain lead the poorest residents to store all the water they can, providing breeding areas for Aedes aegypti. Health authorities must therefore assess each city to establish strategies to combat the disease.
Either way, the action needs to be multifaceted, with vaccines and other means to combat mosquitoes of various kinds. Paolo Zanotto argues that data should be collected redundantly to maximize the efficacy of interventions, with action by governments, universities and the private sector. The integration and dissemination of independently validated information is what could lead to concerted action to prevent epidemics and drives the intervention to save resources. If areas at risk were well known, it would not be necessary, for example, to vaccinate the entire population, says Zanotto. “What I do would have greater impact if there were effective institutional interaction. It’s time to think differently and act in a coordinated manner: without overlap there will be gaps.”
Projects
1. Improvement and evaluation of Aedes aegypti transgenic lines to control dengue transmission (No. 2013/19921-9); Grant mechanism: Regular Research Grant; Principal investigator: Margareth Capurro Guimarães (ICB-USP); Investment: R$310,817.00 (FAPESP).
2. Dengue: production of experimental lots of a candidate tetravalent vaccine against dengue (No. 2008/50029-7); Grant mechanism: Research Program for the Unified Health System (SUS); Principal investigator: Isaias Raw (Butantan Institute); Investment: R$ 1,926,149.72 (FAPESP/CNPq-PPSUS).
3. Phylogeography of the dengue virus in the cities of Jundiaí and Guarujá in São Paulo State (No. 2010/19059-7); Grant mechanism: Regular Research Grant; Principal investigator: Paolo Marinho de Andrade Zanotto (ICB-USP); Investment: R$229,608.82 (FAPESP).
4. Vaccine approaches to the control of dengue fever based on recombinant proteins and microbial-derived adjuvants (No. 2011/51761-6); Grant mechanism: Regular Research Grant; Principal investigator: Luís Carlos de Souza Ferreira (ICB-USP); Investment: R$813,542.17 (FAPESP).
Scientific articles
AMORIM, J.H. et al. The dengue virus non-structural 1 protein: Risks and benefits. Virus Research, V. 181, p. 53-60. March 6, 2014.
ARAUJO, R.V. et al. São Paulo urban heat islands have a higher incidence of dengue than other urban areas. The Brazilian Journal of Infectious Diseases, V. 19, No. 2, p. 146-55. March-April, 2015.
CATELAN, T.B.S. et al. Evaluation of toxicity of phenolic compounds using Aedes aegypti (Diptera: Culicidae) and Artemia salina. Advances in Infectious Diseases, V. 5, No. 1, p. 48-56. February 28, 2015.
CARVALHO, D.O. et al. Two male step release strategy using transgenic mosquito lines to control transmission of vector-borne diseases. Acta Tropica, V. 132 Supplement, p. S170-7. April 2014.
MACORIS, M.L.G. et al. Impact of insecticide resistance on the field control of Aedes aegypti in the State of São Paulo. Journal of the Brazilian Society of Tropical Medicine, V. 47, No. 5, p. 573-8. September-October 2014.
VILLABONA-ARENAS, C.J. et al. Detection of four dengue serotypes suggests rise in hyperendemicity in urban centers of Brazil. PLOS Neglected Tropical Diseases. February 27, 2014.
