In late July, the heads of 19.6 million low-income Brazilian households went to a Caixa Econômica Federal branch, a lottery retailer, or used a mobile app to receive payments from Bolsa Família, one of the world’s largest conditional cash transfer programs. Each household, averaging 2.5 members, received roughly R$671.52. That translates to less than R$9 per person per day—just above the poverty line for the world’s poorest countries, defined by the World Bank as US$3 per person per day (around R$7.50 when adjusted for purchasing power). In upper-middle-income nations like Brazil, the poverty line is higher, at US$8.30 (R$20.92). Yet it’s that modest amount that helps households, largely headed by women, pay for basics like food, housing, and clothing.
Created in 2003, Bolsa Família merged earlier welfare programs and helped reduce poverty and extreme poverty rates across Brazil. Its impact, however, extends beyond household income. Over the past decade, researchers have documented its impact on public health, linking it to declines in premature births, infant mortality, infectious diseases, and even health problems tied to substance dependence.
A recent study, published in The Lancet Public Health in May, analyzed the program’s effect on hospitalizations and deaths across Brazil’s 5,570 municipalities. The findings were impressive: from 2004 to 2019, Bolsa Família directly contributed to preventing an estimated 8.2 million hospitalizations and 713,000 deaths in 3,671 cities for which detailed data were available. The avoided hospitalizations represent at least 70% of those occurring annually within Brazil’s National Healthcare System (SUS). The lives saved between 2004 and 2019 amount to nearly half of all annual deaths in the country.
Researchers reached this conclusion by analyzing birth and death records, including causes of death, from municipal registries and SUS databases between 2000—before Bolsa Família began—and 2019. To estimate its impact, they intersected the share of the target population reached with the average payment per household. Municipalities were classified by coverage level: low (up to 29.9% of the target group), medium (30%–69.9%), high (70%–99.9%), and full coverage, in which all eligible households received benefits. Currently, households earning less than R$218 per person per month qualify for the program. These data were fed into statistical models that also factored in demographic shifts, social and economic progress, improved access to sanitation and healthcare, and earlier social welfare programs.
“We analyzed mortality and hospitalization trends to see whether the declines began only after the program was launched or were already underway. We found that Bolsa Família was the single most influential factor in reducing these rates during the study period,” explains economist Daniella Cavalcanti, lead author of the study and a researcher at the Institute of Collective Health at the Federal University of Bahia (ISC-UFBA).
Between 2004 and 2019, hospitalizations dropped by an average of 31%, and mortality rates fell 25%. During that same period, Bolsa Família expanded dramatically—from covering 50.7% of families living below the poverty line in 2004 to 99.3% in 2019. In municipalities with broad coverage (more than 70% of the target population) and higher payments, hospitalizations fell 22.5% and deaths 27.7%. The effects were most pronounced among the youngest and oldest age groups: mortality dropped by one-third among children under 5, while hospitalizations were cut nearly in half among people over 70 in those communities.
The team used data gathered between 2000 and 2022 to project future trends through 2030, simulating three possible scenarios: reduced coverage, steady coverage, and expanded coverage—where eligibility would extend to families earning less than R$754.50 per person per month (roughly half Brazil’s minimum wage). In the expansion scenario, the model predicts an additional 8 million hospitalizations and 684,000 deaths could be prevented.
Experts note that the program’s health impact stems from more than just income. Bolsa Família’s requirements for continued eligibility help integrate families more fully into Brazil’s public health and education systems. Families receiving the benefit must keep children aged 6 to 17 enrolled in school. Children under 7 must have up-to-date vaccinations and undergo nutritional monitoring to ensure their weight and height are appropriate for their age. Pregnant women are required to attend prenatal care appointments. Noncompliance can result in temporary payment suspensions or removal from the program. As of July, 47,000 families (0.24%) had benefits suspended and 1.1 million had payments blocked—mostly to update their registration details—according to Brazil’s Ministry of Social Development, Family, and Hunger Relief (MDS).
“This century, we’ve seen remarkable improvements in Brazilians’ health—sharp declines in disease and mortality rates, and steady gains in life expectancy. There’s no question that the SUS played a major role in this. But social programs to reduce poverty and extreme poverty have also made a significant contribution,” wrote epidemiologist Maurício Lima Barreto and colleagues in a March report from the Center for Integrated Health Data at the Oswaldo Cruz Foundation (CIDACS-FIOCRUZ), in Bahia.
The internal report—obtained by Pesquisa FAPESP—highlights several positive outcomes linked to Bolsa Família, particularly for women’s and children’s health. The findings draw on analyses of birth, nutrition, illness, and mortality data from tens of millions of Brazilians, shared by the Ministry of Social Development (MDS) with CIDACS and synthesized across 15 scientific papers published in the last five years.
Among those studies: Bolsa Família was associated with a 31% reduction in maternal mortality and a 17% lower risk of death from breast cancer, according to results published in JAMA Network Open in 2024 and 2023, respectively. Researchers also documented a 4% decline in deaths from cardiovascular disease in both men and women, and a 31% reduction in extreme preterm births, defined as those occurring before 28 weeks of pregnancy. The program has additionally been linked to fewer cases and deaths from infectious diseases such as HIV/AIDS and tuberculosis, along with declines in hospital admissions for alcohol- and drug-related disorders and psychiatric conditions.
“The impacts of the program went far beyond what we initially imagined,” says Rômulo Paes de Sousa, a physician and epidemiologist who heads the Center for Strategic Studies (CEE) at FIOCRUZ in Rio de Janeiro. Sousa, a coauthor of the Lancet Public Health study, previously served as secretary for program evaluation and information management at the MDS from 2004 to 2007, where he helped design and implement the program’s monitoring and evaluation framework. “Even without being explicitly designed around gender, the program had a striking impact on women,” he notes.
For children, Bolsa Família helped reduce the risk of stunted growth, though it was also linked to a higher likelihood of overweight and obesity. The risk of death among children under five was at least 17% lower in beneficiary families compared with nonbeneficiaries. Among the children of Black mothers, that reduction reached 26%, according to a 2021 study published in PLOS Medicine.
Despite these gains, researchers point to areas still needing improvement. Teams from the State University of Rio de Janeiro (UERJ) and the Federal University of Rio de Janeiro (UFRJ) analyzed complementary feeding indicators among nearly 507,000 children above six months of age, 44% of whom were receiving Bolsa Família benefits. Their findings, published in 2024 in the International Journal of Environmental Research and Public Health, showed that most nutritional indicators were worse among beneficiary families. In these households, fewer children received solid foods between six and eight months, and meal frequency was lower. Diets were also less varied, with a higher intake of ultra-processed foods. “Among infants under one year old, meal frequency and consumption of foods with adequate consistency, minimum variety, and high iron content were even lower,” says Andreia Andrade-Silva, a nutritionist and the study’s lead author. “Ultra-processed food consumption was high across both groups, but higher among children from beneficiary households. That reflects the historical vulnerability of low-income households,” adds Maria Beatriz de Castro, a nutritionist and epidemiologist at UFRJ, a coauthor of the study and Andrade-Silva’s doctoral advisor.
The health benefits of income-transfer programs for children aren’t unique to Brazil. A field experiment involving 10,000 families in 653 villages across Kenya, conducted by researchers from the UK and the US, found that giving families direct cash payments—without any conditions attached—helped reduce child mortality. A one-time transfer of US$1,000 was linked to a 48% drop in deaths during the first year of life and a 45% decline in deaths by age five, according to a paper published in August in the NBER Working Papers series. The researchers noted, however, that the effect faded once the cash transfers stopped.

Marcelo Camargo / Agência BrasilFamilies receiving Bolsa Família must keep children aged 6–17 enrolled in schoolMarcelo Camargo / Agência Brasil
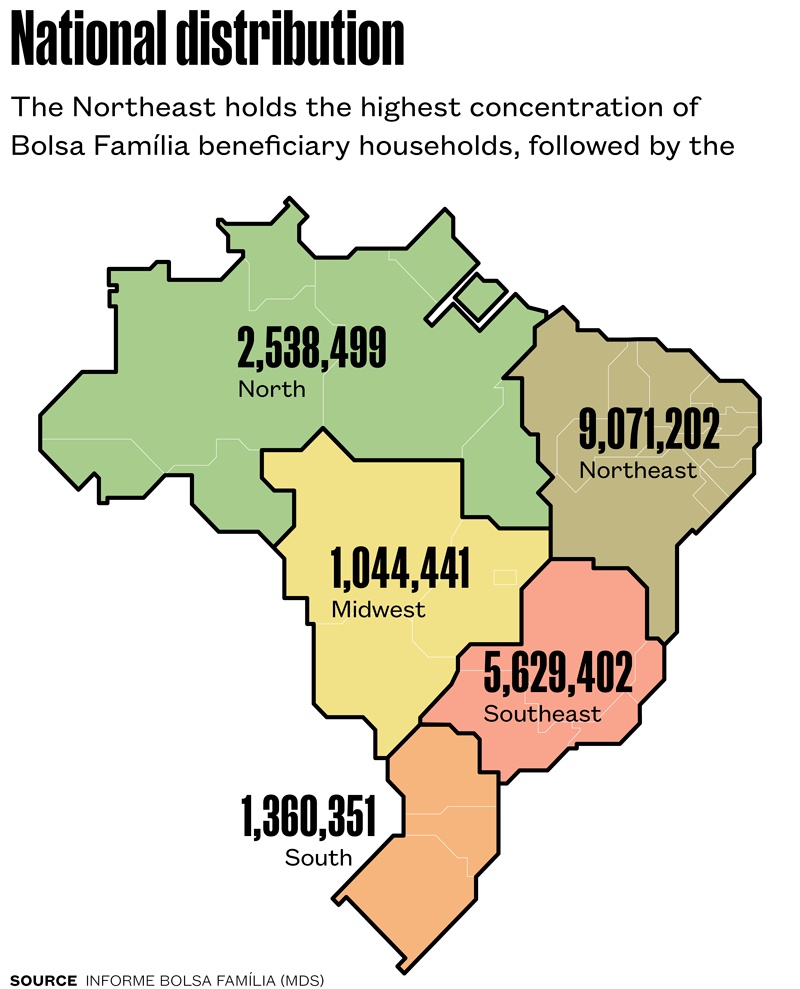
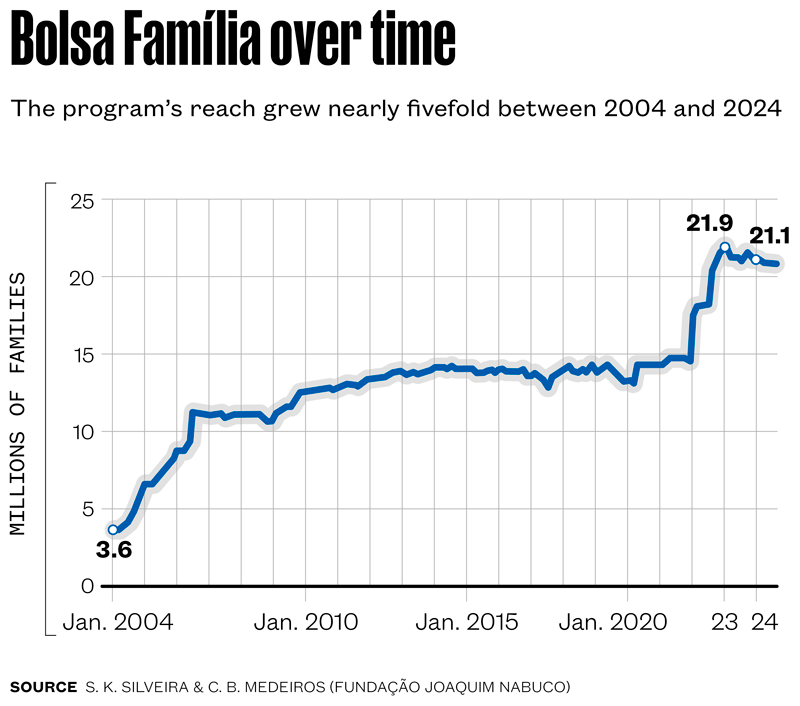
Inspired by international initiatives—particularly Mexico’s pioneering Programa de Educación, Salud y Alimentación (Progresa/Oportunidades)—Brazil launched Bolsa Família through Provisional Order No. 132 in October 2003, later enacted as Law N° 10,836 the following year. The program’s first payments reached 1.15 million families. Since then, Bolsa Família has gone through periods of rapid growth, stability, and renewed expansion. Its budget has risen from 0.3% of Brazil’s GDP in 2004 to roughly 1.5% in 2024. In January 2023, the program hit a record 21.9 million participating families, before entering a phase of gradual decline (see chart). As of July 2025, the Northeast remained the region with the largest share of beneficiaries, followed by the Southeast (see map).
Critics have argued that Bolsa Família might discourage formal employment by prompting workers to stay in informal jobs to preserve benefits. But according to Brazil’s General Register of Employed and Unemployed Workers (CAGED), program beneficiaries and former beneficiaries filled 76% of the 1.69 million formal-sector jobs created in 2024. A recently updated transition rule, introduced in July, allows families whose income rises above R$218 per person per month to continue receiving half their benefits for one additional year.
The program still faces major challenges. One persistent issue is ensuring that families in remote regions can access both the program benefits and the education and healthcare services required to meet the program’s eligibility conditions. “Unfortunately, regional inequalities in Brazil are profound, and there are what we call government service voids—areas far from primary healthcare services,” explains epidemiologist Ethel Maciel, of the Federal University of Espírito Santo (UFES), who served in Brazil’s Ministry of Health until early 2025.
“While Bolsa Família does provide essential support, it’s a solution at the household level that doesn’t address the structural roots of poverty,” says Alessandro Pinzani, an Italian philosopher at the Federal University of Santa Catarina (UFSC) and coauthor of Vozes do Bolsa Família: Autonomia, dinheiro e cidadania (Voices of Bolsa Família recipients: Autonomy, money, and citizenship; Editora Unesp, 2013). For Pinzani, tackling poverty’s deeper causes requires different strategies: in cities, it requires addressing inequality and the low pay for manual labor; in rural areas, it requires expanding access to land. “Those changes,” he notes, “are not easy to accomplish in the short term.”
The story above was published with the title “Income and health” in issue 355 of September/2025.
Scientific articles
CAVALCANTI, D. M. et al. Health effects of the Brazilian conditional cash transfer programme over 20 years and projections to 2030: A retrospective analysis and modelling study. The Lancet Public Health. July 2025.
GUIMARÃES, J. M. N. et al. Income segregation, conditional cash transfers, and breast cancer mortality among women in Brazil. JAMA Network Open. Jan. 25, 2024.
ALVES, F. J. O. et al. Association of conditional cash transfers with maternal mortality using the 100 million Brazilian cohort. JAMA Network Open. Feb. 23, 2023.
PESCARINI, J. M. et al. Impact of Brazil’s Bolsa Família Programme on cardiovascular and all-cause mortality: A natural experiment study using the 100 million Brazilian cohort. International Journal of Epidemiology. Dec. 2022.
SILVA, A. F. et al. Intersectional impact of cash transfers on Aids among 123 million Brazilian women. Nature Human Behavior. Aug. 11, 2025.
JESUS, G. S. et al. Effects of conditional cash transfers on tuberculosis incidence and mortality according to race, ethnicity and socioeconomic factors in the 100 million Brazilian cohort. Nature Medicine. Jan. 3, 2025.
FALCÃO, I. R. et al. Brazil’s Bolsa Família conditional cash transfer and child malnutrition: A Nationwide birth cohort study. The BMJ Global Health. July 20, 2025.
RAMOS, D. et al. Conditional cash transfer program and child mortality: A cross-sectional analysis nested within the 100 million Brazilian cohort. PLOS Medicine. Sept. 28, 2021.
ANDRADE-SILVA, A. et al. Trends in complementary feeding indicators in children aged 6-23 months according to participation in a conditional cash transfer program: Data from the Brazilian food and nutrition surveillance system, 2015-2019. International Journal of Environmental Research and Public Health. July 15, 2024.
WALKER, M. W. et al. Can cash transfers save lives? Evidence from a large-scale experimente in Kenya. NBER Working Paper Series. Aug. 2025.
