From the end of January until the beginning of March, almost 22 million inhabitants in 77 municipalities of São Paulo, Rio de Janeiro, and Bahia are expected to receive the fractionated yellow fever vaccine (a fifth of the full dose); this is considered the best strategy to halt the epidemic of wild-transmitted yellow fever, which has caused 907 cases and 314 deaths across the country between June 2016 and January 2018. The decision by the Brazilian Ministry of Health to fraction the vaccine, which was announced in early 2018, mainly stems from the fact that it is impossible to give a full dose to all inhabitants in risk zones and areas where the disease-causing virus is expected to arrive in the coming months.
In 2017, the Technological Immunobiological Institute (Bio-Manguinhos), a unit of the Oswaldo Cruz Foundation (FIOCRUZ) in Rio de Janeiro and the only Brazilian manufacturer of the vaccine, expanded monthly production from 4 million to 6 million doses and ceased exports, prioritizing the domestic market. Even so, production has not been sufficient to keep pace with the spread of sylvatic yellow fever. Since November 2016, the virus that causes the disease (which is transmitted by mosquitoes in the genera Haemagogus and Sabethes that live in wild areas) has progressed at an unexpectedly rapid rate through regions in Minas Gerais, Espírito Santo, São Paulo, and Rio de Janeiro which had previously been considered free of the disease and where residents for the most part had not been vaccinated.
Long queues in front of vaccination stations in large cities at the beginning of January, before the intensive vaccination campaign began, indicated the population’s concerns; people sought the whole-dose vaccine when possible, thinking that the fractionated vaccine might not be as effective. In order to contribute to the debate on the current strategy for combating the epidemic, Pesquisa FAPESP interviewed a number of experts and presents the scientific basis for using the vaccine in this form. In summary, fractioning is backed by scientific studies and is thought to protect against the virus, but there is uncertainty about the effectiveness and duration of this protective effect, as well as controversy over the need for booster doses.
The fractionated vaccine
Three controlled clinical trials demonstrated positive results for the immunogenicity (the ability to activate the body’s defenses) of the fractionated vaccine. The first was conducted by Bio-Manguinhos in 300 soldiers aged 18–47 and published in 1988 in the Journal of Biological Standardization. The second was performed in the Netherlands by a team from the University of Leiden, in 175 people aged 25–27; it was published in PLOS ONE in 2008, and showed that 1/5 of the normal dose had the same protective effect as the standard dose. The final study was done by FIOCRUZ in Rio de Janeiro in 749 soldiers with a mean age of 19.4 years. The participants were divided into six groups; each received a different dose, since the study investigated the effectiveness of the vaccine in six distinct concentrations: 1/1 (whole) and fractions of approximately 1/3, 1/10, 1/60, 1/170, and 1/900 of the standard dose. The results, published in 2013 in Human Vaccines & Immunotherapeutics and in 2014 in BMC Infectious Diseases, indicated that concentrations as low as 1/10 of the original dose preserved the protective effects against the virus which were induced by the standard dose.

Ascom / Bio-Manguinhos / Fiocruz
At Bio-Manguinhos, the yellow fever vaccine has been produced using essentially the same technique involving embryonated eggs since 1937Ascom / Bio-Manguinhos / FiocruzLower doses also caused production of antibodies, which alone is not sufficient to stop the virus, observes biochemical pharmacist Olindo Assisi Martins Filho, researcher at the René Rachou Institute, a unit of FIOCRUZ in Minas Gerais. He states that better immunogenic response involves balanced production of antibodies, defense cells, and mediators known as interleukins which activate defense cells, stimulate the production of antibodies, and more broadly regulate the body’s defenses against the microorganisms that cause diseases (see table on page 49).
All three tests in humans had limitations. In a July 2016 document, the World Health Organization (WHO) noted that the number of participants and the age range were restricted, preventing more comprehensive conclusions. For this reason, children up to 2 years of age, pregnant women, people who have undergone organ transplants, patients with autoimmune diseases, or adults over age 60, who were not represented in these studies, will continue to receive the standard vaccine. In a large-scale study, researchers from Imperial College London compared the results of 12 clinical trials conducted between 1965 and 2011 which involved a total of 4,868 people. “As detailed in a 2016 article in the American Journal of Tropical Medicine and Hygiene, the 1/10 dose generated a response equivalent to 97% of the standard dose, which was measured by the production of virus-neutralizing antibodies.”
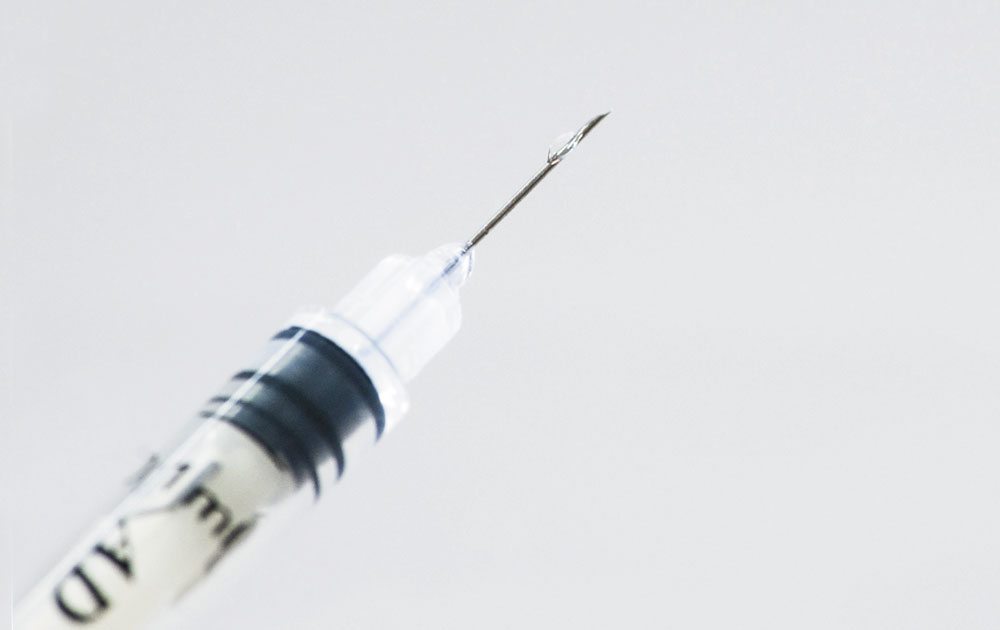
“We are absolutely assured about the effectiveness of fractioning,” says veterinarian Akira Homma, senior scientific adviser for Bio-Manguinhos. Fractionated doses can vaccinate up to 25 people in the areas where the virus has not yet arrived (but may soon reach) using 5 standard doses, since each person receives 0.1 milliliter (ml) doses instead of the 0.5 ml standard dose via special syringes. “With the 4 million doses we have, we will be able to immunize everyone,” he adds.
Homma states that in 2013, pressure from the lack of the vaccine led the WHO to approve fractioning (also 1/5 of the full dose) to stop an epidemic of a different type of yellow fever in Africa, the urban variety transmitted by the Aedes aegypti mosquito. “It worked very well,” says Homma. Approximately 30 million people were vaccinated in emergency campaigns in Angola and the Democratic Republic of the Congo. The outbreak that began in December 2015 in Angola ended in February 2017, after causing 965 deaths in the two countries.

Léo Ramos Chaves
Fractioning allows one 5-dose vial to vaccinate up to 25 people in areas the virus has still not reachedLéo Ramos Chaves“The dose equivalent to 1/5 of the full dose will protect the same,” reiterates infectologist Marcos Boulos, coordinator for disease control at the São Paulo State Secretary of Health (SES-SP) and professor at the University of São Paulo School of Medicine (FM-USP). Physician and physicist Eduardo Massad partly disagrees. “The fractionated vaccine is immunogenic, but nobody knows if it is really effective. We have only indirect evidence that it is, since until this time yellow fever has not reemerged in Angola and the Democratic Republic of the Congo,” observes Massad, a professor at FM-USP.
Massad’s questioning is based on two arguments. The first is that the efficacy of the lower-concentration doses was not evaluated in animal models, which receive the vaccine followed by the virus to determine the actual degree of protection and most effective dosage. The second argument is that the results are not guaranteed: the dengue vaccine presented good results in initial clinical trials in healthy people, but performed poorly during the next stage, in vaccinated people who were then infected with the virus. “It is one thing to produce antibodies, another to not catch the disease,” adds Massad. The body’s response may vary from person to person, and in some cases may not be enough to stop the virus.
It is also not known whether the reactions will be equal to those of the standard vaccine. “It is assumed that the reactions are equivalent, but the fractioned vaccine was not evaluated in the population on a large scale,” adds Massad. After the 2009 outbreak of yellow fever in Botucatu, São Paulo, with 29 confirmed cases and 11 deaths, he coordinated the plan to expand areas of vaccination in the state, as described in a 2015 article in the Memórias do Instituto Oswaldo Cruz [Memoirs of the Oswaldo Cruz Institute]
In January, health authorities said that only people traveling in areas of risk for transmission of sylvatic yellow fever should be vaccinated. This was one way to prioritize vaccination of residents of these areas, where mosquitoes infected with the virus circulate, and to avoid the risk that undesirable side effects from the vaccine might eclipse the disease itself. In São Paulo, three individuals under 60 years of age died in early 2018 from reactions to the vaccine. According to the Department of Health, some did not report prior diseases that would have barred them from immunization.
 Uncertain duration
Uncertain duration
Another question remains unanswered: how long is the protective effect of the fractioned vaccine expected to last? In January 2018, doctors, researchers, and health authorities stated that the fractionated 1/5 dose could sustain protection against the virus for at least eight years, but this information was based on a study which is not yet complete and has not yet been published by researchers from FIOCRUZ in Rio de Janeiro and Minas Gerais.
In 2017, the FIOCRUZ team sought out the participants in the second study, which evaluated the effect of fractionated doses in soldiers in Rio through measuring immunogenicity, in order to see how long the vaccine’s protection extended. But the year when the participating soldiers received the vaccine, which should have been the starting point in assessing the duration of the protective effects, was not included in the 2013 and 2014 articles. Martins Filho, who participated in the second article and is part of the study by the new team, says that the fractionated doses were applied in 2009. Of the 749 soldiers who participated in the previous study, 319 were located, said they had not been revaccinated, and agreed to participate in the new study. According to FIOCRUZ, analysis of blood samples indicated that the majority of the reevaluated men had maintained high levels of the virus-neutralizing antibodies and memory cells.
The biochemical pharmacist Alejandro Costa, a researcher at the WHO’s Initiative for Vaccine Research, learned the results of the new FIOCRUZ study in December 2017 at a meeting at the Ministry of Health in Brasília. “The evidence on the duration of the protective effect in the FIOCRUZ study seems consistent, but has not been validated by a committee of experts,” he observes. He says that during this meeting, one of the WHO’s recommendations to the FIOCRUZ teams and the states that will adopt the fractionated vaccine was to monitor representative samples of the population over the coming years to effectively observe the duration of the fractionated dose’s protective effect.

Léo Ramos Chaves
In São Paulo (above) and in other large cities, the advance of the epidemic has led to long lines in front of vaccination stationsLéo Ramos ChavesBooster doses?
How long the protective effects of the whole dose last is also uncertain. “I do not believe it lasts a lifetime,” says Marcos Boulos, who recalled a meeting at the Ministry of Health in 1983. In this meeting, experts said that the vaccine, which at the time was recommended for 10 years, could last for at least 30. In 2013, when the WHO was faced with a shortage of vaccines to tackle the epidemic in Africa, it changed the recommendations and stated that a single dose lasted not only 10 years, but for a person’s entire life. The Brazilian Ministry of Health adopted this guideline in 2017.
“At this time, according to the current guidelines, there is no need for booster doses,” says physician Helena Sato, director of immunization at SES-SP. In a 2013 article in the American Journal of Tropical Medicine and Hygiene based on 36 studies on immunogenicity in adults, children, and pregnant women, researchers from the Alexander von Humboldt Institute of Tropical Medicine in Peru and the WHO concluded that protective effects could extend throughout life, ruling out the need for a booster dose. But this point is also controversial. Based on a study by FIOCRUZ in Minas Gerais published in 2016 in Human Vaccines & Immunotherapeutics, Martins Filho argues that the effect begins to drop five years after the first vaccine and becomes critical after 10 years, when 70% of vaccinated people retain the ability to react to the virus, justifying a booster dose.
“I was at the WHO meeting in 2013 and opposed the decision for the single dose,” says virologist and physician Pedro Vasconcelos, director of the Evandro Chagas Institute in Belém. “It is more prudent to vaccinate at least twice, because not all people respond the same way.” In a commentary in the February 2018 edition of the Memórias do Instituto Oswaldo Cruz, he defended the need for a booster dose and more modern vaccines against yellow fever. Bio-Manguinhos is one of four manufacturers recognized by the WHO, who argue that the low cost of the dose impedes investments in expansion and new production methods. The vaccine has essentially been produced the same way since 1937: a specific strain of the yellow fever virus is passed through embryonated eggs dozens of times until it weakens, inducing the production of antibodies and memory cells that attack the normal virus if it appears in humans.
Vaccination protects people, but does not stop the transmission of the virus by mosquitoes
FIOCRUZ in Pernambuco is researching an immunization prepared from the virus’s genetic material, and expects to test new formulations as soon as possible. Meanwhile, FIOCRUZ in Rio is working on a model based on the inactivated yellow fever virus. The two studies are still far from any conclusions. In an article published in 2011 in the New England Journal of Medicine, a team from the Xcellerex company in the United States reported that a vaccine produced using a deactivated virus proved to be safe and immunogenic in a study with 60 people aged 18–49. GE Healthcare Life Sciences acquired the rights to the Xcellerex vaccine in 2012, and sold them to another pharmaceutical company, PnuVax, in 2016. The tests continue.
Risk of expansion
Even though the vaccination campaigns and the fractionated doses are demonstrating the desired results, yellow fever has become endemic in most Brazilian states and in neighboring countries: it has already reached parts of Argentina, Bolivia, Paraguay, Peru, Colombia, Ecuador, and Venezuela. “Might it be possible to eradicate an outbreak of sylvatic yellow fever after it erupts, through mass vaccinations?” asked physician Caio de Souza Manso, head of the vaccination department of the Ministry of Health’s National Yellow Fever Service, in 1957. “We believe not, or, at least, we have not achieved it.” His arguments are still relevant, six decades later. The vaccination protects people, but does not interrupt the cycle of virus transmission: infected mosquitoes will continue to bite monkeys that live in the forest and serve as temporary hosts for the virus. When other mosquitoes bite these wild primates, they acquire the virus and eventually pass it on to people who have not been vaccinated that live in or visit forested or jungle areas.

WHO / E. Soteras Jalil
Health clinic on the outskirts of Kinshasa, the capital of Congo, during the vaccination campaign to stop the 2016 epidemicWHO / E. Soteras JalilMassad is troubled by the possibility that urban yellow fever may return; this disease is transmitted by Aedes aegypti and was last recorded in Brazil in 1942. “If Aedes increases numerically in outlying areas and bites infected monkeys and then people, it will be a tragedy.” Two studies published in Scientific Reports in 2017 support this possibility. In the first, a team from the USP School of Public Health found that Aedes mosquitoes are predominant in nine public parks in the city of São Paulo. In the second, a team from FIOCRUZ Rio, the Pasteur Institute in France, and the Evandro Chagas Institute noted that Aedes is just as capable of carrying the yellow fever virus as Haemagogus and Sabethes. “The number of Aedes in cities is currently low, but may increase,” warns the WHO’s Costa. “We must intensify preventive vaccination to prevent urban yellow fever, which is more difficult to control than sylvatic.”
Scientific articles
ROUKENS, A. H. et al. Intradermally administered yellow fever vaccine at reduced dose induces a protective immune response: A randomized controlled non-inferiority trial. PLOS ONE. v. 3, n. 4, e1993. 2008.
MARTINS, R. M. et al. A double blind, randomized clinical trial of immunogenicity and safety on a dose-response study 17DD yellow fever vaccine. Human Vaccines & Immunotherapeutics. v. 9, p. 879–88. 2013.
CAMPI-AZEVEDO, A. C. et al. Subdoses of 17DD yellow fever vaccine elicit equivalent virological/immunological kinetics timeline. BMC Infectious Diseases. v. 14, p. 391. 2014.
OMS. Fractional dose yellow fever vaccine as a dose-sparing option for outbreak response. 2016.
LOPES, O. de S. et al. Studies on yellow fever vaccine III — dose-response in volunteers. Journal of Biological Standardization. v. 16, n. 2, p. 77-88. abr. 1988.
MONATH, T. P. et al. An Inactivated Cell-Culture Vaccine against Yellow Fever. The New England Journal of Medicine. v. 364, n. 14, p. 1326-33. 7 abr. 2011.
JEAN, K. et al. A Meta-Analysis of Serological Response Associated with Yellow Fever Vaccination. American Journal of Tropical Medicine and Hygiene. v. 95, n. 6, p. 1435-9. 7 dez. 2016.
RIBEIRO, A. F. et al. A public health risk assessment for yellow fever vaccination: a model exemplified by an outbreak in the state of São Paulo, Brazil. Memórias do Instituto Oswaldo Cruz. v. 110, n. 2, p. 230-4. abr. 2015.
GOTUZZO, E. et al. Efficacy and Duration of Immunity after Yellow Fever Vaccination: Systematic Review on the Need for a Booster Every 10 Years. American Journal of Tropical Medicine and Hygiene. v. 89, n. 3. p. 434-44. 4 set. 2013.
VASCONCELOS, Pedro FC. Single shot of 17D vaccine may not confer life-long protection against yellow fever. Memórias do Instituto Oswaldo Cruz. v.113, n. 2, p.135-7. fev. 2018.
CAMPI-AZEVEDO, A. C. et al. Booster dose after 10 years is recommended following 17DD-YF primary vaccination. Human Vaccines & Immunotherapeutics. v. 12, n. 2, p. 491-502. fev. 2016.
MANSO, C. de S. Vacinação em massa contra a febre amarela no Brasil. Boletim de la Oficina Sanitaria Panamericana. v. 43, n. 4, p. 341-55. 1957.
MEDEIROS-SOUZA, A. R. et al. Mosquitoes in urban green spaces: using an island biogeographic approach to identify drivers of species richness and composition. Scientific Reports. v. 7, n. 1, 17826. 19 dez. 2017.
COUTO-LIMA, D. et al. Potential risk of re-emergence of urban transmission of Yellow Fever virus in Brazil facilitated by competent Aedes populations. Scientific Reports. v. 7, n. 1, 4848. 7 jul. 2017.