As people live longer, concern grows—both for themselves and for their families—about the onset of neurodegenerative diseases, particularly Parkinson’s and Alzheimer’s, which together affect more than 400 million people worldwide. The former causes tremors, muscle stiffness, slowness of movement, pain, sleep disturbances, and, in advanced stages, dementia. The latter is characterized by memory loss, difficulties with reasoning, orientation, and language, as well as behavioral changes and loss of autonomy. Although more common in older adults, these diseases affect the functioning of the brain and other parts of the central nervous system and are not considered a natural part of aging. Of complex origin, they often result from the interaction between genetic predisposition and exposure to environmental factors that increase the risk of developing them.
Seeking to identify possible ways to reduce this risk, an international team of researchers, including one Brazilian scientist, decided to look beyond the brain, the structure where damage is concentrated once Parkinson’s or Alzheimer’s takes hold. They also investigated problems and changes that occur in other organs and tissues long beforehand, which may influence the vitality and functioning of the central nervous system.
In a study published in August in the journal Science Advances, the team led by Spanish pharmacist and neuroscientist Sara Bandrés-Ciga, then head of neurogenetics at the Center for Alzheimer’s and Related Dementias at the US National Institutes of Health (NIH), evaluated how 155 conditions affecting the digestive and metabolic systems could influence the risk of developing Parkinson’s or Alzheimer’s. These 155 diseases were selected because they involve the structures of the so-called gut–brain axis, a network of organs and glands in the digestive tract that, in various ways, affect the functioning of the central nervous system. The reverse is also true—brain activity can influence how these structures perform.
The researchers found that four of these health conditions were associated with up to a threefold increase in the risk of developing Parkinson’s disease, and 13 others with a higher likelihood of developing Alzheimer’s (see infographic on page 62). All of these conditions typically develop years before the first symptoms of either neurodegenerative disease appear. Type 1 and type 2 diabetes, as well as intestinal disorders such as irritable bowel syndrome, were shown to be linked to an increased risk of developing both Alzheimer’s and Parkinson’s.
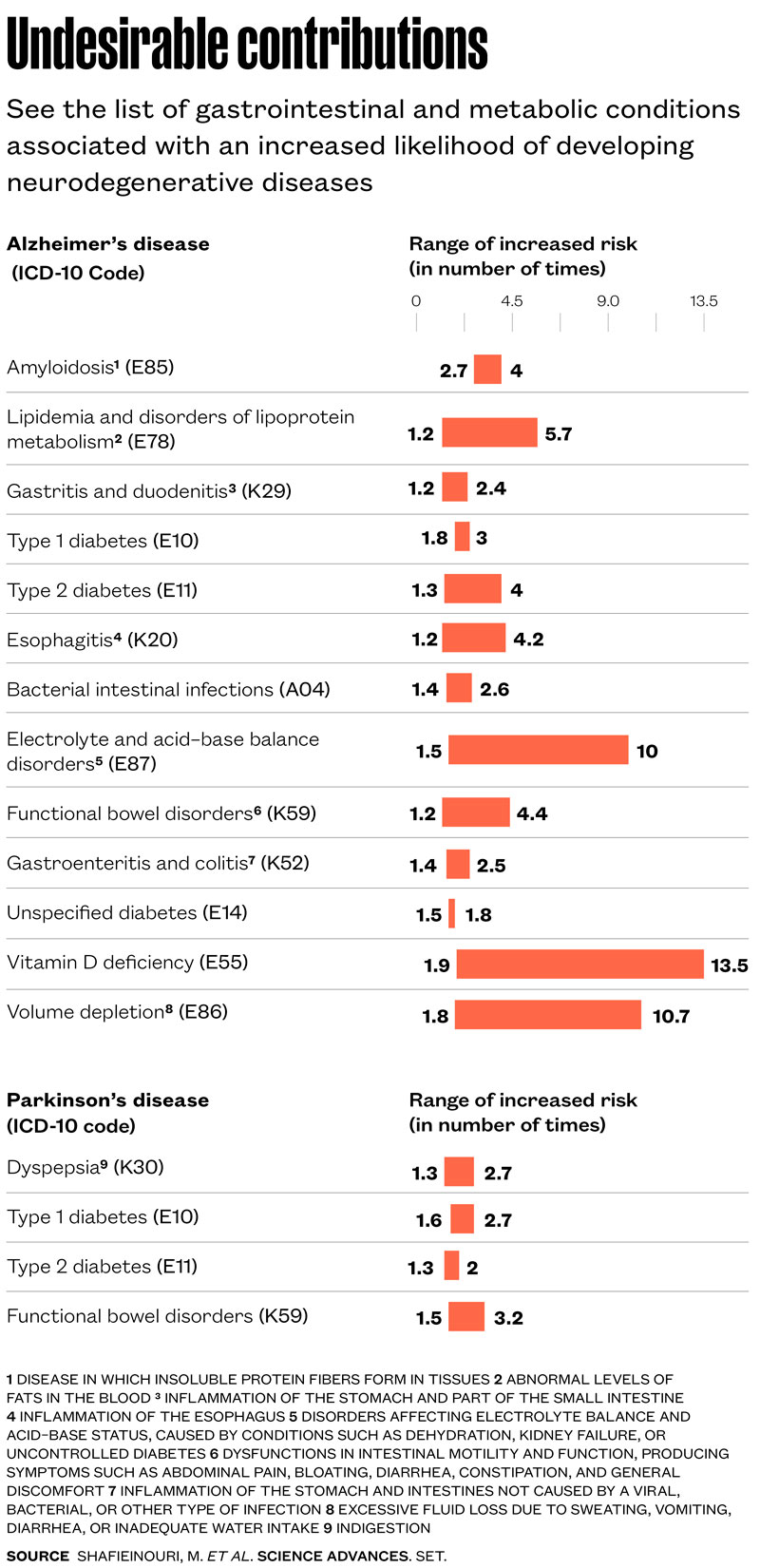
“In the case of Alzheimer’s, problems related to fat metabolism, vitamin D deficiency, mineral imbalances, and inflammation of the digestive tract, such as esophagitis, gastritis, and colitis, also stood out,” says Bandrés-Ciga, who now works at the biotechnology company Valo Health, in an interview with Pesquisa FAPESP. “Issues such as chronic indigestion, pancreatic dysfunction, and B-complex vitamin deficiencies were associated with an increased risk of Parkinson’s disease.”
The researchers emphasize that these findings do not establish a causal relationship—that is, they do not prove that conditions such as diabetes cause Parkinson’s or Alzheimer’s. However, the fact that digestive and metabolic problems tend to appear long before the onset of neurodegenerative diseases suggests that they may contribute to their development.
“The hypothesis is that these digestive and metabolic disorders may influence the progression of Parkinson’s and Alzheimer’s,” explains Brazilian neurologist Artur Schumacher Schuh, from the Federal University of Rio Grande do Sul (UFRGS), a coauthor of the study. Among the results, he highlights the increased risk linked to type 2 diabetes, which can appear 10 to 15 years before Alzheimer’s. “Diabetes is known to raise cardiovascular risk, and there are indications that it may cause protein glycation [the binding of sugars to proteins, which makes them toxic] and that this process could contribute to the buildup of beta-amyloid plaques characteristic of Alzheimer’s.”
Multiple connections
Previous studies have suggested that inflammation, imbalances in the gut microbiota, or nutritional deficiencies may trigger signals that impair brain function. “There is evidence that malformed proteins, such as those associated with Parkinson’s disease, may even originate in the gut and migrate to the central nervous system via the vagus nerve,” notes Bandrés-Ciga.
“The gut and brain communicate in various ways,” explains immunologist Lício Velloso, from the University of Campinas (UNICAMP), who was not involved in the study. The gastrointestinal system contains neurons and glial cells that interact with the same types of cells found in the central nervous system. One connection pathway is neural, mediated by the vagus nerve, which links the digestive tract to the brain and helps regulate satiety. Another is hormonal, through compounds produced in the stomach and intestines that modulate appetite. A third involves substances synthesized by the gut microbiota (bacteria and other microorganisms living in the intestine) that can enter the bloodstream and influence brain function. “This set of mechanisms, which has been more clearly described in recent years, shows how deeply interconnected the digestive and nervous systems are,” says Velloso, coordinator of the Center for Research on Obesity and Comorbidities at UNICAMP, one of the Research, Innovation, and Dissemination Centers (RIDCs) funded by FAPESP.
To assess the contribution of digestive and metabolic disorders to the risk of developing Parkinson’s and Alzheimer’s, the researchers analyzed genetic, age, and health data from 225,000 people in the United Kingdom who were followed between 1999 and 2023. All were adults and healthy at the beginning of the study, with information stored in the UK Biobank health database, and all had a low genetic risk of developing neurodegenerative diseases. Over the follow-up period, 4,473 participants developed Alzheimer’s disease and 4,564 developed Parkinson’s disease. To validate their findings, the results were compared with data from two other databases containing the health records of tens of thousands of individuals.
Using genetic information and circulating proteins in the blood, the researchers developed a mathematical model capable of predicting the risk of developing Alzheimer’s disease with 90% accuracy and Parkinson’s with 78%. “These numbers are promising, but they still require validation,” explains Schuh, from UFRGS. “The model suggests that it may be possible to estimate an individual’s likelihood of developing these neurodegenerative diseases and, perhaps, identify people who could benefit from early interventions to reduce that risk.” According to Bandrés-Ciga, it is still necessary to “test this tool in more diverse populations, incorporate environmental and lifestyle factors, and address the possibility of false positives” before it can be used in clinical practice.
The possible link between metabolic and digestive disorders and neurodegenerative diseases opens the door to preventive strategies, such as dietary adjustments and the management of intestinal problems and diabetes, before neurological symptoms appear, potentially lowering the risk of Parkinson’s and Alzheimer’s. Despite this encouraging outlook, there is still no conclusive evidence that these measures are effective. “Observational studies suggest protective effects from drugs like metformin and semaglutide, used to treat diabetes, but clinical trials conducted so far have produced mixed results,” says Bandrés-Ciga.
Proportion was estimated based on an analysis of health data from 9,900 people aged over 50
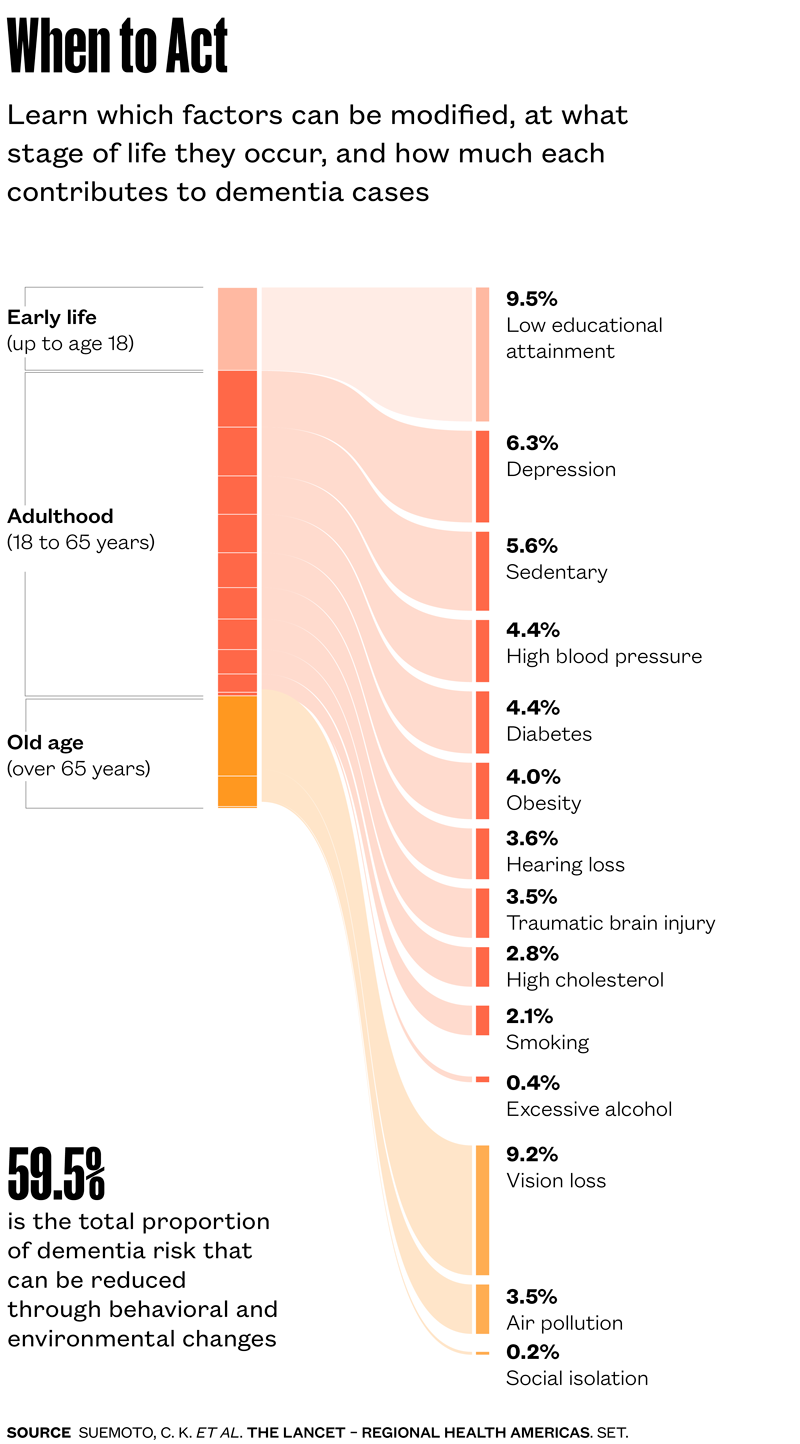
While the Science Advances study raises concerns by suggesting that common illnesses may increase the risk of neurodegenerative diseases, research conducted in Brazil offers a more encouraging perspective. Published in the September issue of The Lancet Regional Health – Americas, the study led by geriatrician Claudia Suemoto from the University of São Paulo (USP) indicates that almost 60% of dementia cases, including Alzheimer’s disease, could be prevented in Brazil if 14 risk factors were fully controlled.
The researchers reached this figure by calculating, based on health data from 9,949 people aged 50 or older who participated in the Longitudinal Study of Health in Brazilian Older Adults (ELSI-Brasil), how much each of the 14 risk factors contributed to the development of dementia. Since 2017, The Lancet’s Commission on Dementia Prevention, Intervention, and Care has listed these factors, which increased from 12 to 14 in 2024 with the addition of reduced visual acuity and high cholesterol levels. Each factor carries a different weight, determined by the strength of its association with dementia and its prevalence in the population. The proportion of dementia cases that could be prevented globally, based on data from high-income countries, is lower than in Brazil, at 45% (see Pesquisa FAPESP issue n° 346).
In Brazil, the factors that most influence the risk of developing dementia are low educational attainment, associated with 9.5% of cases; untreated vision loss, responsible for 9.2%; and depression in middle age, responsible for 6.3% (see infographic). The total potential reduction in dementia cases was similar across different ethnic groups and regions of the country: 59.5% overall, and slightly higher among women (61.1%) than men (58.2%). In a previous version of this estimate, published in 2022, Suemoto’s group calculated that 48.2% of cases could be prevented—or up to 54% in the poorest regions of the country—by addressing 12 risk factors (see Pesquisa FAPESP issue n° 329).
“We cannot rely solely on studies from wealthy countries,” cautions Suemoto. “In Brazil, low educational attainment is the main risk factor for dementia because it remains very common among older adults. In the United States, the average level of formal education is 12 years, and in Europe, 16. Here, the average among the elderly is just five years.”
The story above was published with the title “Before the problem arises” in issue 356 of October/2025.
Scientific article
SHAFIEINOURI, Mohammad et al. Gut-brain nexus: Mapping multimodal links to neurodegeneration at biobank scale. Science Advances. Aug. 27, 2025.
