 MEDICALRF.COM / GETTYIMAGESPublished in may 2011
MEDICALRF.COM / GETTYIMAGESPublished in may 2011
For three decades, cell therapy has successively been a source of enthusiasm and deception for patients suffering from Parkinson’s disease, an illness characterized by the progressive death of the neurons responsible for the production of an important chemical substance, the neurotransmitter dopamine. In the 1980s, a controversial approach to the disease, which initially seemed promising, was tested on animals and even human beings in countries such as Sweden, the United States and México: the transplanting of cells extracted from the adrenal gland or immature brain tissue of aborted fetuses. The rationale underlying these surgeries, which were debatable even from the ethical point of view, was to supply the brain structure known as black substance (which was damaged in the patients because of the progressive loss of dopaminergic neurons) with a new population of cells capable of producing the neurotransmitter. In this way the main symptoms of Parkinson’s, such as tremors, muscular rigidity, slowness of movements and speaking and writing difficulties, should be eliminated. The results of the approach were disappointing. In cases where there was an improvement in the well-being of the patients it was short-lived. In others, not even this occurred, and the attempted treatment even worsened the disease, leading to the death of some individuals.
A group of biologists and neuroscientists from São Paulo may have discovered one of the reasons for the failure of these old cell treatments for Parkinson’s and perhaps understood why the more modern and refined versions of this type of experimental treatment, now based on the use of the so-called stem cells, are still yielding inconsistent results. The transplants tested in pre-clinical studies in laboratory animals may contain a significant number of fibroblasts, a type of skin cell that is very like stem cells, but that has totally different properties.
On April 19, researchers from the University of São Paulo (USP) and from the Federal University of São Paulo (Unifesp) published a study in the on-line issue of Stem Cell Reviews and Reports showing that in rats with induced Parkinson’s, the presence of human fibroblasts cancels out the possible positive effects of implanting mesenchymal stem cells obtained from the tissue of the umbilical cord of newborns.
“When we administered just stem cells the symptoms of the disease in the rats improved,” says geneticist Mayana Zatz, one of the authors of the article and coordinator of the Human Genome Studies Center at USP, one of the Centers of Research, Innovation and Dissemination (Cepid) funded by FAPESP, and the National Institute of Stem Cell Science and Technology in Human Genetic Diseases. “But when we also injected fibroblasts, the beneficial effects disappeared and there was even some deterioration. It’s possible that many poor results in scientific work with cell therapy are due to this type of contamination.” According to the researchers, the work is the first to show both the positive effects of using mesenchymal stem cells against Parkinson’s as well as the harmful effects of contamination by fibroblasts in the same animal model.
In addition to presenting an advance in basic knowledge on the possible benefits of cell therapies in an organ as complex and delicate as the brain, the result of the study is a warning to the families of people with Parkinson’s. In no country in the world is there any officially approved treatment based on stem cells for combating this or any other neurodegenerative disease. “Stem cell research needs to be looked at carefully and false promises of a cure mustn’t be made,” says the author of the article, the neuroscientist Esper Cavalheiro, from Unifesp, who heads the work at the National Institute of Translational Neuroscience, a joint project of FAPESP and the Ministry of Science and Technology (MCT). “Before proposing therapy we need to understand the entire differentiation mechanism of stem cells in the various tissues in the organism and understand what the brain does to “talk to” and direct the operation of these cells.” So far, the only diseases that have stem cell-based treatment are blood diseases, especially cancers (leukemia). Against this type of problem doctors have for decades resorted to the transplant of bone marrow, rich in hematopoietic stem cells, which are the precursors of blood.
Still lacking a cure, Parkinson’s is currently controlled with the help of medication, like levodopa, that the brain can convert into dopamine. In more serious cases, there is a second alternative: to implant electrodes in the brain of patients that are not responding well to the treatment, or who have many side effects from the drugs. Linked to a small generator implanted under the skin, the electrodes try to improve communication between the neurons. The delicate surgery for implanting the electrodes is known as deep brain stimulation, or simply DBS. With the exception of these two approaches, all other procedures against the disease are still in the trial stage and have not been approved by the medical authorities.

Rodrigo A. Bressan/ UNIFESPImage of a normal brain with more neurons that produce dopamine (left) and of anther brain, affected by Parkinson’sRodrigo A. Bressan/ UNIFESP
Dopamine, a chemical messenger produced by less than 0.3% of the nerve cells, belongs to a class of substances called neurotransmitters, whose basic function is to pass information on from one neuron to another in the form of electrical signals. This communication process between neurons is known as synapse. Dopamine acts specifically on brain centers linked to the sensations of pleasure and pain and has a proven role in the mechanisms that generate dependence and addiction and also the control of movement. In the case of Parkinson’s victims, the motor issue is clearly affected due to the lack of the neurotransmitter.
It is very easy to mix up fibroblasts and mesenchymal stem cells and this confusion may be at the heart of the inconclusive or contradictory results of many attempts at treating Parkinson’s with cell therapies. Both types of cell have the same origin. They derive from the mesenchyme, the main connective tissue of the embryo, from which various types of cell will form. Despite their common origin, fibroblasts and mesenchymal stem cells have different properties. Responsible for the synthesis of collagen, fibroblasts form the basis of the connective tissue in an adult individual. They are, therefore, specialized, differentiated cells. Mesenchymal stem cells, on the other hand, are very non-differentiated and can generate many types of tissue, such as bone, cartilage, fat, support cells for the formation of blood and connective fibrous tissue. “It’s almost impossible to distinguish these two types of cells if we simply examine them under a microscope,” comments the biochemist Oswaldo Keith Okamoto, from the Human Genome Studies’ Center, and coordinator of the article published in Stem Cell Reviews and Reports. “They grow in vitro under the same conditions and we only distinguish them with the help of markers and specific tests.” Mesenchymal stem cells also have an important peculiarity. They have immunosuppressive properties and can reduce the need to take medication to avoid the rejection of transplanted organs and tissues.
There is no hard evidence that mesenchymal stem cells can generate the neurons that are lacking or somewhat dysfunctional in Parkinson’s disease patients. Still, they seem to improve the environment in which the lesions associated with disease occur, reduce local inflammation and favor the preservation of more nerve cells. “Their effects might be indirect, reducing the inflammation in the brain,” says Okamoto. This is what the researchers from São Paulo saw in their experiment with rats. They injected stem cells into the brain of a group of ten rodents with induced Parkinson’s and one month later found that they had no symptoms of the disease. They were as healthy as the animals in the healthy control group. This result coincides with the conclusions of similar studies conducted both here and abroad.
What was really new happened in the second part of the experiment. The scientists inserted a culture of fibroblasts into another group of ten rats, also with Parkinson’s. The result was a disaster. A month after the procedure the animals started exhibiting more motor problems and the number of dopaminergic neurons in the black substance dropped by half. A third group of sick rodents was given a mixture of two types of cell, in equal parts. In this group, no improvement whatsoever was seen. It is as if the fibroblasts cancelled out the apparently beneficial effects of the stem cells. “They seem to be neurotoxic,” says Mayana.
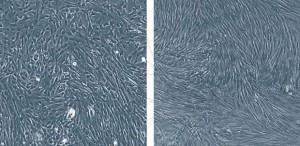
Mariane SeccoMesenchymal stem cells (left) and fibroblasts: difficult to distinguish between themMariane Secco
In India, a group of doctors and scientists from the BGS-Global Hospital, in Bangalore, is testing the use of mesenchymal stem cells in seven human patients aged 22 to 62 who are suffering from Parkinson?s. Obtained from the bone marrow of the patients themselves, the cells were injected into the damaged brains in accordance with a local protocol created by the Indians. In an article published in February of last year in Translational Research, the researchers reported a reduction in the symptoms of the disease in three of the seven patients and said that the approach seemed safe. The results, however, are still preliminary and must be viewed with reservation. “Mesenchymal stem cell transplants may not become a definitive treatment for Parkinson’s, but perhaps a complementary one, like neuroprotection,” Okamoto considers. “This type of study can help us understand how to mitigate the degenerative environment in the brain and maybe how to create new drugs against the disease; who knows?”
Genes, environment and mystery
Although there are cases of young individuals with Parkinson’s, such as the famous Canadian actor, Michael J. Fox, who was diagnosed at the age of 30, this neurological disorder appears more often in people older than 50 or 60. “Patients under 50 are seen as precocious and represent some 20% of the total,” says the neurologist Luiz Augusto Franco de Andrade, from the Teaching and Research Institute at the Albert Einstein Hospital in São Paulo. “But I’ve already treated a boy of 13 who had Parkinson’s.”
There is growing evidence that environmental and genetic factors may be implicated in the appearance of the disease, at least in some cases. A study by Harvard Medical School researchers, published in October of last year in Science Translational Medicine, showed that hundreds of genes linked to the functioning of the mitochondria, organelles that are the organism’s power plant, are less active in Parkinson’s patients. Even people who are in the initial stage or even pre-Parkinson’s seem to have these changes. If this connection between the mitochondria and the disease is confirmed, drugs that act on these genes may become useful in treating the problem.
Twice as many patients by 2030
Along a similar line of investigation, a study published in September 2010 by the National Institutes of Health (NIH) of the United States suggested that individuals with a certain version of the GRIN2A gene might benefit more from the consumption of coffee and tea. In a person with this genetic profile, the intake of beverages containing caffeine might act as a protection factor against Parkinson’s. The search for substances that help to maintain neurons is a strategy adopted by many research groups. Administering the GDNF protein, which acts in this way, has been the target of tests for years, to check its possible action against the disease.
Despite localized advances in our understanding of the possible mechanisms implicated in its genesis, Parkinson’s still maintains its general status of a neurodegenerative disease whose cause is both mysterious and unexplained. No one knows for certain why the neurons that produce dopamine begin to die or stop functioning correctly at a particular point in the life of certain people. The only concrete thing known is a palpable fact of the current reality: an ageing population is a great risk factor for Parkinson’s. This issue is of particular concern to developing nations, whose age structure is rapidly changing before they become rich.
Still seen as a nation of young people, Brazil’s demographic profile will change dramatically over the next few decades. A report from the World Bank published last month points out that its 65 or older population will rise from the current 11% to 49% by 2050. In a period of 40 years, the number of old people will triple. It will leap from fewer than 20 million to around 65 million. “The speed of population ageing in Brazil will be significantly greater than that in more developed societies in the last century,” say those responsible for the report Envelhecendo num Brasil bem mais velho [Growing old in an older Brazil]. In France it took more than a century for the population of 65 years or older to increase from 7% to 14% of the total. “Over the last few years, modern gerontology has emphasized the increase of the ageing process more than its physical and mental losses,” says anthropologist Guita Grin Debert, from the State University of Campinas (Unicamp), who studies issues linked to women and old age. “We have experts in diseases but not many in the ageing process.”
A review study published in January 2007 in the scientific journal Neurology analyzed data divulged in a further 62 pieces of work and concluded that the number of cases of Parkinson’s in people over 50 should double over the next 20 years in 15 countries around the globe. The work analyzed statistics from the world’s most highly populated nations, including Brazil, and the five biggest in Europe. In 2005, this group of countries had between 4.1and 4.6 million patients with Parkinson’s. In 2030, it will have between 8.7 and 9.3 million cases of the disease. In this same period, the number of those with it in Brazil will leap from 160,000 to 340,000. According to the scientific article, the estimated growth rates of the incidence of Parkinson’s in developing countries such as China, India and Brazil, whose populations are only now undergoing an ageing process, will be over 100%. In developed economies, which already have a large number of old people, such as Japan, Germany, Italy and the United Kingdom, the number of sick people should increase by less than 50%.
 Instituto Santiago Ramón y Cajal / WikimediaIn broad terms, it is estimated that 1% of the planet’s inhabitants over 65 is likely to suffer from Parkinson’s disease. However, this figure may vary according to the characteristics of the population analyzed. A study conducted in 2006 in Bambuí, in Minas Gerais, found a high incidence of Parkinson’s: more than 7.2% in a group of 1,186 individuals over 64. This figure is three or four times higher than that found in similar work carried out in Europe, Asia and the United States. Almost half the cases of the disease in Bambuí had been caused by the uncontrolled use of drugs against psychoses and dizziness. “We currently believe that the number of cases of the disease arising from the uncontrolled use of drugs has decreased,” says Francisco Cardoso, from the Federal University of Minas Gerais (UFMG), coordinator of the study. “Control of the sale of drugs in the country has improved.”
Instituto Santiago Ramón y Cajal / WikimediaIn broad terms, it is estimated that 1% of the planet’s inhabitants over 65 is likely to suffer from Parkinson’s disease. However, this figure may vary according to the characteristics of the population analyzed. A study conducted in 2006 in Bambuí, in Minas Gerais, found a high incidence of Parkinson’s: more than 7.2% in a group of 1,186 individuals over 64. This figure is three or four times higher than that found in similar work carried out in Europe, Asia and the United States. Almost half the cases of the disease in Bambuí had been caused by the uncontrolled use of drugs against psychoses and dizziness. “We currently believe that the number of cases of the disease arising from the uncontrolled use of drugs has decreased,” says Francisco Cardoso, from the Federal University of Minas Gerais (UFMG), coordinator of the study. “Control of the sale of drugs in the country has improved.”
Stem cells are not science’s only bet to improve treatments for Parkinson’s. There are no prospects of a cure in the short-term. However, researchers hope that it will be possible to bar the evolution of this neurological disturbance, or at least retard its progress, by developing new drugs and more effective and, if possible, less invasive surgery. “At present, we try to offset the effects of Parkinson’s by administering oral medication,” says Cardoso. “But the way in which we replace dopamine is not good.” When, for example, the patient takes the drug levodopa, a precursor of dopamine, his brain comes into contact with high concentrations of the neurotransmitter. As time passes, the amount of the substance drops. Consequently, the treated patient experiences cycles of excess and shortage of the neurotransmitter, a sort of chemical seesaw, with dopamine highs and lows.
Some drugs try to regulate the moment at which dopamine, produced artificially via the ingestion of levodopa, becomes available for use by the brain of the sick person. However, control of this process still needs to be refined and imitation of the physiological mechanism is imperfect. The situation becomes even more complicated when the drugs no longer control Parkinson’s symptoms or produce side effects. The prolonged use of dopamine precursors sometimes causes involuntary and repetitive movements, technically called dyskinesia, which may cause patients to bite their lips, poke their tongue out or blink rapidly. In these cases, deep brain stimulation (DBS) surgery may be indicated.
Two years ago the team of the Brazilian neuroscientist Miguel Nicolelis, from Duke University (USA) and founder of the Edmond and Lily Safra International Institute of Neurosciences of Natal (IINN-ELS), suggested that electrical stimulation might produce good results against Parkinson’s, without the need to open up the heads of patients. In an article that was on the cover of the scientific journal Science in March 20, 2009, Nicolelis reported a successful experiment on rats and mice with induced Parkinson’s: the installation of small electrodes on the surface of the spinal medulla of the animals helped them recover their normal locomotion capacity. According to the scientist, the procedure for placing the electrodes takes 20 minutes, is not very invasive (only the skin of the animal is cut) and is safe. The new approach, which is now being tested on monkeys, was the first attempt at treating Parkinson’s without acting directly on the brain.
It is difficult to forecast whether new Parkinson’s treatments will arise from studies such as those of the teams of Mayana Zatz, at USP, and Esper Cavalheiro, at Unifesp. For the time being this work, as well as that of other scientists, still comprises lines of research that should be explored rather than immediate treatment possibilities. Nonetheless, doctors who care for people with Parkinson’s see no reason for pessimism. Patients are living for an increasingly long time with the disease, even decades, although there is the delicate issue of the side effects of the medication. Still, the electrodes and batteries used in DBS surgery are becoming smaller and more efficient. “We still don’t know how the neurons “talk” to each other, but today we can record the activity of a larger number of brain cells,” says the neurosurgeon Manoel Jacobsen Teixeira, a professor at USP and a member of the Institute of Teaching and Research at the Sirio-Libanês Hospital in São Paulo.
Scientific articles
1. PEREIRA, M. C. et al. Contamination of mesenchymal stem cells with fibroblasts accelerates neurodegeneration in an experimental model of Parkinson’s disease. Stem cell reviews and reports. Published online on April 19, 2011.
2. VENKATARAMANA, N. K. et al. Open-labeled study of unilateral autologous bone-marrow-derived mesenchymal stem cell transplantation in Parkinson’s disease. Translational Research. v. 155 (2), p. 62-70. Feb. 2010.