ArchaeaAssociation of bacteria: possible cause of inflammation of the arteriesArchaea
For many years, atherosclerosis was defined as the gradual build-up of fatty materials in the artery walls. Low-density lipoproteins (LDL), a kind of fatty material, became famously known as the bad cholesterol, responsible for the mechanism that can lead to myocardial infarction and cardiovascular disease, the main cause of death around the world. In the last few years, the explanations have become more refined and atherosclerosis has begun to be viewed as a chronic inflammatory process, which feeds on and is fed by the deposition of fat in the artery walls. This approach is now flourishing in Brazil in the form of three new treatment possibilities that have produced positive results in preliminary tests conducted on animals.
The treatment currently at the most advanced stage was developed at the Instituto do Coração/InCor heart institute, linked to the University of São Paulo/USP. It consists of anti-tumor drugs that are expected to produce effects on inflammatory processes; testing these drugs on human beings is scheduled to begin this year. Another experimental treatment with this same approach – atherosclerosis viewed as an inflammation – is being conducted by researchers from the State University of Campinas/Unicamp, and has shown promising results, to the point that the researchers have already attracted the interest of a Brazilian pharmaceutical company interested in participating in the tests, which are protected by contractual non-disclosure. The third possibility, also developed by InCor, is based on the presupposition that atherosclerosis could be generated or made worse by groups of microorganisms, with the participation of archaea, representatives of the earliest strains of microorganisms to appear on our planet. This presupposition was the basis of the experimental use of an enzyme produced by the Trypanosoma cruzi protozoa, which causes Chagas disease, to eliminate bacteria and archaea found in the fatty plaques that block the flow of blood.
As these experiments mature, they may come to complement the most popular treatment at this time, which is based on drugs called statins. These drugs reduce the quantity of cholesterol and can have an additional effect by helping control inflammation, according to recent studies. New treatments may also reduce the impact of atherosclerosis, which can lead to cardiovascular diseases, the leading cause of death in world, especially when combined with high blood pressure and smoking. The fatty plaques with dead blood cells that are slowly deposited in the artery walls can obstruct the flow of blood which distributes oxygen to all of the cells in the body. These fatty plaques, called atheroma, can jeopardize the functioning of vital organs, such as the heart, causing myocardial infarction, or the brain, provoking a stroke. According to the World Health Organization/WHO, cardiovascular diseases kill approximately 15 million people every year around the world, which corresponds to 30% of the total number of deaths every year. In Brazil alone, approximately 350 thousand people a year suffer heart attacks, the most serious heart condition of all.
“There is a lack of new drugs for atherosclerosis”, says endocrinologist Raul Maranhão, a researcher at InCor and professor at the Medical School and at the Pharmaceutical School of the University of São Paulo/USP. The possibility of treatment that he devised consists of adjusting artificial spheres of lipids (fat) with a diameter of 30 to 60 nanometers, which he began to develop 15 years ago, with cancer drugs that also help stop the proliferation of defense cells on the inflamed walls of the arteries. Called LDE, the acronym for cholesterol-high emulsion, these spheres simulate the low-density lipoprotein molecules/LDLs that are naturally produced by the body. After verifying that these artificial fatty particles stayed in places where cells with accelerated proliferation were found, such as tumors and inflamed tissues, Maranhão placed a pharmaceutical component, called paclitaxel – normally used in cancer therapy – into the fatty spheres. Then he injected these spheres into rabbits and fed the rabbits with high-fat foods for a period of two months. According to an article published in April 2008 in the journal Atherosclerosis, the sphere with the paclitaxel reduced lesions in the arteries by 60% – caused by altered versions of cholesterol – even in the cases of rabbits whose cholesterol levels in the blood were 200 times above the normal level. The sphere also reduced the migration of the macrophages – the defense cells that intensify the inflammatory process – to the artery walls.
 “I found the key to enter the cell”, says Maranhão. To evaluate whether the artificial cholesterol spheres actually traveled to the sites of intense cell growth, he added technetium, a radioactive chemical element, to the spheres and injected them into people. As expected, the tumors absorbed twice as much cholesterol as the normal cells. In 2002, the researcher conducted the initial safety tests on 46 people using the spheres with the anti tumorals. According to him, the pharmaceutical compound encapsulated by the fatty capsule became five to eight times less toxic than the isolated pharmaceutical compound, because of the affinity of rapidly growing cells with fat, which is badly needed by such cells. Tests conducted on approximately one hundred people indicated that this procedure was safe and the tests conducted on the rabbits reinforced his argument to propose the use of these spheres, with a drug normally used in cancer therapy, to treat atherosclerosis as well.
“I found the key to enter the cell”, says Maranhão. To evaluate whether the artificial cholesterol spheres actually traveled to the sites of intense cell growth, he added technetium, a radioactive chemical element, to the spheres and injected them into people. As expected, the tumors absorbed twice as much cholesterol as the normal cells. In 2002, the researcher conducted the initial safety tests on 46 people using the spheres with the anti tumorals. According to him, the pharmaceutical compound encapsulated by the fatty capsule became five to eight times less toxic than the isolated pharmaceutical compound, because of the affinity of rapidly growing cells with fat, which is badly needed by such cells. Tests conducted on approximately one hundred people indicated that this procedure was safe and the tests conducted on the rabbits reinforced his argument to propose the use of these spheres, with a drug normally used in cancer therapy, to treat atherosclerosis as well.
In a calm manner, Maranhão comments, in his office at InCor, that a treatment that began to be evaluated as a therapy for cancer can now be tested as therapy for atherosclerosis, because both diseases have one characteristic in common – the intense proliferation of cells. This similarity between two diseases is supported by a line of research which began with an article published in January 1999 in the New England Journal of Medicine by physician and pathologist Russell Ross, a professor at the US’s Washington University. “Atherosclerosis is an inflammatory disease”, Ross stated – he was the only author of this article. He argued that: “Due to high concentrations of LDL, viewed as one of the main risk factors in atherosclerosis, the atherogenesis process (the formation of fatty plaques), has been considered the result of the build-up of lipids in the walls of the arteries; however, it is much more than this”. Ross showed that the increase of lipid levels and of altered lipoproteins, in addition to other blood molecules such as homocysteines, as well as infection and high blood pressure, may induce or provoke inflammation associated with atherosclerosis. “This work changed the view on atherosclerosis, which nowadays is considered as being chronic inflammation”, says Maranhão.
Ross died two months later, at the age of 69. He did not live to see that his work also motivated the research teams working at pharmaceutical companies to seek new drugs for the treatment of atherosclerosis. One of the companies that entered this race, US company AtheroGenics, announced in March 2008 the beginning of the final stage of the clinical trials of AGI-1067, its main candidate for this kind of drug, that may help stop the buildup of sugars and fats; this is why this compound will also be tested – beginning this year – for diabetes therapy. Research work by pharmaceutical companies is normally conducted quietly, even when the work is done in collaboration with universities.
This is also the case, in Brazil, of a compound with the potential to be used in inflammatory disease therapy, such as atherosclerosis and arthritis. The compound is the result of a six-year research project that was part of the doctorate studies of Silvana Rocco at Unicamp’s School of Medical Sciences. The compound acts on a specific group of enzymes that are involved in the inflammatory process. Preliminary tests have attested to the compound’s therapeutical potential and have attracted a Brazilian pharmaceutical company, which is expected to participate in the compound’s final evaluations, conducted under contractual non-disclosure. According to physician Kleber Franchini, who coordinates the team at Unicamp, the company is also financing the compound’s patent filings in other countries and is expected to finance the clinical trials on human beings, scheduled to begin this year or next.
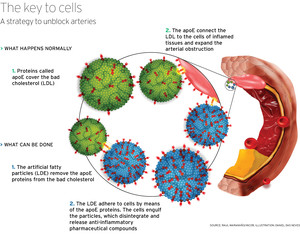 The third treatment possibility goes back to the deepest origins of atherosclerosis. The problem starts when a cholesterol molecule infiltrates itself into the walls of the arteries and undergoes a chemical reaction – oxidation – which attracts the macrophages, the defense cells. The macrophages engulf the oxidized cholesterol and form the so-called foam cells, which attract more lipids. This forms a foreign body inside the organism that other defense cells will try to destroy by means of inflammatory processes that inflate the walls of the veins and arteries and block the flow of the blood. Fat can also start building up as a result of physical injuries to the walls of the blood vessels.
The third treatment possibility goes back to the deepest origins of atherosclerosis. The problem starts when a cholesterol molecule infiltrates itself into the walls of the arteries and undergoes a chemical reaction – oxidation – which attracts the macrophages, the defense cells. The macrophages engulf the oxidized cholesterol and form the so-called foam cells, which attract more lipids. This forms a foreign body inside the organism that other defense cells will try to destroy by means of inflammatory processes that inflate the walls of the veins and arteries and block the flow of the blood. Fat can also start building up as a result of physical injuries to the walls of the blood vessels.
Physician and pathologist Maria de Lourdes Higuchi, a researcher at InCor and a professor at USP’s Medical School, has come up with another possibility: in her opinion, the inflammation associated with atherosclerosis might be generated by groups of microorganisms with the participation of archaea. She resorted to this hypothesis, which has not been fully proved yet, to develop an experimental treatment based on an enzyme of the Trypanosoma cruzi protozoa.
The hypothesis of the associations of microorganisms being the cause of atherosclerosis came up when Maria de Lourdes was trying to understand why the same person could have two types of atherosclerosis plaques on the walls of the arteries. One type of plaque grows, bursts, and releases particles of fat that block the blood vessels and cause myocardial infarction; another type basically consists of stable plaques, with less fat and more fibers, that do not burst. While examining fragments of 13 coronary arteries with plaques that had burst, Maria de Lourdes detected, by means of genome analysis, microorganisms of the archaea group among the bacteria – especially the Chlamydophila pneumoniae and Mycoplasma pneumoniae, which have this name because they can cause pneumonia. Other researchers had already found Chlamydophila and Mycoplasma on the fatty plaques, but it was not clear what kind of role they played. Maria de Lourdes believes that these microorganisms, once they come together, may cause inflammation by interacting with fat by means of a chemical reaction called oxidation, which leads to fat buildup.
Resistant to the point of surviving in extreme environmental conditions such as acid sea water or in the midst of volcano lava, the archaea had not yet been associated with diseases in humans. However, according to Maria de Lourdes, they can produce enzymes that annul the actions of the defense cells. Thus, she says, “the archaea are able to survive and let the surrounding bacteria also survive and multiply”. The other microorganisms might also contribute to this group’s well-being by forming a pool of bacteria: the Chlamydophila pneumoniae, inhibiting the programmed death of host cells, and the Mycoplasma pneumoniae, by their own mechanisms, also dodging the organism’s defense mechanisms.
The arguments that she and her team from InCor presented in 2006 in Clinics, a Brazilian scientific journal, helped explain other issues. Maria de Lourdes believes that superoxide dismutase, one of the enzymes produced by archaea, might be responsible for breaching the outer collagen layer of the plaques, releasing particles of fat that can clog the arteries, such as the ones that irrigate the heart, and provoke a heart attack. The reasons for the movements of the defense cells into the inflamed tissue and the poor efficiency of antibiotics to reduce the incidence of heart attacks in patients with atherosclerosis became somewhat clearer. “The antibiotics don’t eliminate archaea”, points out Maria de Lourdes.
Based on this evidence, she created an unusual strategy to break up this microbe club. The strategy is unusual because it implies using an enzyme called transialidase, produced by the Trypanosoma cruzi protozoa. Maria de Lourdes noticed that the arteries of people who had died of Chagas disease did not have atheroma. After verifying that the mycoplasma adhere to regions of the artery wall that contain sialic acid, the same acid that this enzyme transfers to the protozoa, she prepared a solution with the enzyme and other compounds able to inhibit the action of the archaea and injected it into rabbits that had been fed high-fat food.
“The transialidase reduced the number of fatty plaques and, with other compounds, dropped the cholesterol in the blood back to normal levels”, she said. According to her, the results, detailed in 2004 in the Medical Hypotheses journal, open up the possibilities of using the strategy in other diseases as well. “Many tumoral cells seem to be high in archaea and mycoplasma”, says Maria de Lourdes. Other specialists are viewing her work hopefully. “New causes do not exclude existing causes”, says Maranhão.
Researchers who discover new treatment possibilities have to deal with two challenges: convince their demanding colleagues that they discovered something important and produce the compounds which, they believe, will solve many problems. Maranhão spent many years looking for companies which could produce the artificial fat spheres able to transport drugs against tumors and inflammation. In view of unsuccessful agreements, he concluded that he himself would have to expand the scale of production.
Maranhão worked for two years with his team to move on from a simple production method to the current production method, which uses a compressor able to produce 50 doses of the solution with the spheres and the compound inside in 30 minutes. This is enough leeway to conduct an evaluation of the efficacy of this approach on 40 people, provided that his plans are approved by the committees of the InCor. Franchini was luckier; four years ago, when he was looking for partners, he found colleagues and companies willing to help. “We learned the way”, he says. “Here at Unicamp we now have people doing the research and who are also attuned to the development of the pharmaceutical components. We are beginning to realize that we can produce other new things”. Maria de Lourdes, on the other hand, is still looking for interested parties.
Even if new anti-inflammatory drugs able to detain atherosclerosis come onto the market a few years from now, statins will still be used. One of the reasons is that statins, in addition to reducing cholesterol levels, can reduce the quantity of C reactive proteins, associated with inflammation, according to a study conducted on approximately 18 thousand people (men at the age of 50 or over and women at the age of 60 or over, with normal cholesterol levels), conducted by AstraZeneca, a company that produces statins. The findings were divulged last year. High cholesterol levels are still the main risk factor for atherosclerosis, but other indicators are beginning to attract attention. “High levels of homocysteine in the blood are linked to atherosclerosis”, says Franchini, “but we don’t know whether this is the cause or the consequence”.
The projects
1. Lipid nanoparticles: investments in the study of the physiopathology, diagnosis and therapy of degenerative diseases (nº 06/58917-3); Modality Theme Project; Coordinator Raul Cavalcante Maranhão – InCor; Investment R$ 1.401.712,38.
2. Pathogenesis of hypertrophy and heart failure: mechanisms activated by mechanical stimulus (nº 06/54878-3); Modality Theme Project; Coordinator Kleber Gomes Franchini – Unicamp; Investment R$ 996.638,13.
3. Biomolecular study of products of Chlamydia pneumoniae and Mycoplasma pneumoniae in the progression of chronic valvular heart disease in humans (nº 07/04067-1); Modality Regular Research Awards; Coordinator Maria de Lourdes Higuchi – InCor; Investment R$ 100.882,40.