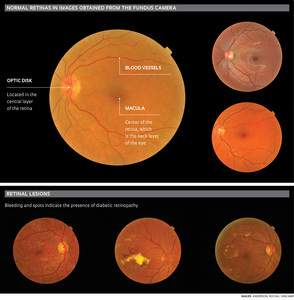
 An essential need for patients with diabetes is to identify whether or not they have diabetic retinopathy, an eye disease that can lead to blindness. The risk increases if glycemic control is inadequate and the patient is not examined by an ophthalmologist. Diagnosis is performed by mapping the retina or by analyzing color photographs produced by a device called a fundus camera. To aid in this analysis and make diagnoses quicker, researchers from the Institute of Computer Science at the University of Campinas (IC-Unicamp) developed a computational solution that can aid in the detection and treatment of the disease. The software is able to automatically analyze images of the retina — at the back of the eye — in diabetic patients and indicate abnormalities such as bleeding, vascular changes, scars and signs of inflammation early on.
An essential need for patients with diabetes is to identify whether or not they have diabetic retinopathy, an eye disease that can lead to blindness. The risk increases if glycemic control is inadequate and the patient is not examined by an ophthalmologist. Diagnosis is performed by mapping the retina or by analyzing color photographs produced by a device called a fundus camera. To aid in this analysis and make diagnoses quicker, researchers from the Institute of Computer Science at the University of Campinas (IC-Unicamp) developed a computational solution that can aid in the detection and treatment of the disease. The software is able to automatically analyze images of the retina — at the back of the eye — in diabetic patients and indicate abnormalities such as bleeding, vascular changes, scars and signs of inflammation early on.
This innovation is important because the disease is the leading cause of blindness in the working population — aged 20 to 74 — in developed countries. “According to the International Diabetes Federation, the disease currently affects 366 million people worldwide, and this number is expected grow to approximately 552 million by 2030,” says project coordinator Professor Anderson Rocha, IC-Unicamp. In Brazil, an estimated nearly 5% of the population, or close to 10 million Brazilians, are diabetic, some of whom may develop diabetic retinopathy. For now, the software only works on ordinary computers, but the plan is to develop a portable fundus camera and equip it with the new system, in partnership with specialized companies at some time in the future An ophthalmologist or even a nurse could capture the image of the patient’s retina. “Diabetics who live in rural or remote communities would benefit greatly if a portable device was developed and brought to them,” says Rocha. “In this way, a nurse could determine if the patient needed to see a physician.” The device could also detect the disease in its early stages, an essential step towards preventing blindness. In addition, a portable fundus camera would be faster and leave more time for the ophthalmologist to examine patients.
The software works in four steps: assessment of image quality, detection of lesion, screening, and verification of the need for treatment. “It is able to recognize errors in image capture, such as when the image is of a part of the retina that is not considered ideal for detecting retinopathy or even if the patient blinks,” says computer scientist Ramon Pires, a doctoral student on Rocha’s team.
Assured the minimum image quality for analysis, the individual detectors of lesions associated with diabetic retinopathy perform an analysis. The patient’s retinal image passes through six lesion detectors in the software, and each of them gives the image a score that indicates the probability of a patient having a lesion. “The image becomes represented to a high degree by a set of numbers, one for each lesion, and this new representation allows the physician to check if the patient has problems associated with diabetic retinopathy, if the disease is in an advanced stage, and if the patient needs to schedule an appointment with an ophthalmologist during the following 12 months,” explains Rocha. Among the signs and lesions that indicate diabetic retinopathy and that can be detected by the software are the presence of fat, red lesions, light and heavy bleeding, cotton-like spots and microaneurysms. “We achieved classification results above 90% in recent studies, consistent with the best results in the scientific literature,” Rocha says.
Support group
The research that led to the software began in 2009 with a project funded by the partnership between the Microsoft Research Institute and FAPESP, under the supervision of Professor Jacques Wainer, also from IC-Unicamp. In 2011, the work received additional support from the Foundation, in that case for Pires’ master’s degree work, and Samsung became involved during the second half of 2013. In addition to Rocha and Pires, the group includes Professors Siome Goldenstein and Wainer, from IC, and Eduardo Valle, of the Unicamp School of Electrical Engineering and Computer Science.
“This software can be of great assistance in diagnosing diabetic retinopathy,” said physician Sérgio Gianotti Pimentel, a professor in the Department of Ophthalmology at the School of Medicine of the University of São Paulo (USP). “Several similar programs have been reported in the literature,” he says. The same applies to portable fundus cameras. “Recently, some researchers have begun to take an interest in this line of research,” says Rocha. “However, we’re not aware of any work in progress on automated portable devices like the one we intend to develop. We’re seeking partnerships and just signed one with the Unicamp Hospital de Clínicas.”
Project
Automated screening for diabetic retinopathies: IT in the fight against preventable blindness (nº 2008 / 54443-2); Grant Mechanism Regular Line of Research Project Award – Microsoft agreement, Coord. Jacques Wainer/Unicamp; Investment R$ 176,198.75 and $ 75,855.79 (FAPESP).