 UNIVERSITY OF WISCONSIN / MADISON
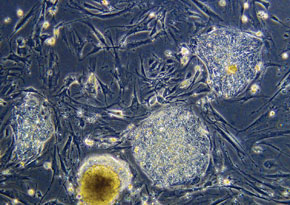
UNIVERSITY OF WISCONSIN / MADISONHuman ESCs: more difficult to manipulate than mouse cellsUNIVERSITY OF WISCONSIN / MADISON
Stem cells, which can produce different body tissues, have attracted the interest of scientists and the population in general because they represent a possibility of treatment for health problems that still lack satisfactory treatments. Tests conducted in different countries in the last few years have confirmed the versatility of these cells – especially of the embryonic stem cells (ESCs), extracted from the embryo a few days after it is formed – and have led to a surge of optimism, which, however, seems exaggerated for the time being.
The more scientists study these cells, the more they discover that there is still a lot that needs to be done before stem cells can be used in new therapies. “I would be afraid of injecting stem cells into my body and even more afraid of using induced pluripotent stem cells (iPS), regarding which many questions still have no answers,” says Joshua Brickman, from the Centre for Regenerative Medicine of Scotland’s University of Edinburgh. “We have to continue the research studies,” he states. Brickman was in Brazil last March, working on the final items for the fourth “Embryonic stem cells as a model system for embryonic development” course, scheduled to take place in 2013 at the Center for Studies on the Human Genome of the University of São Paulo.
The course, which is divided into theory and practice, will bring together the world’s foremost specialists on stem-cell research with researchers at the beginning of their careers for a period of three weeks. Brickman and Jennifer Nichols, a researcher at the University of Cambridge’s Center for Stem Cell Research, in England, developed this initially itinerant course seven years ago to train young researchers from Latin America. The course has already been held in Chile, Mexico, and Brazil. Now, Brickman and Jennifer intend to establish a permanent base in one of these countries.
Read the main excerpts, below, from their interview to Pesquisa FAPESP , during which they talked about the course and about issues linked to embryonic stem cells (ESCs).
Why don’t we know how to maintain pluripotent ESCs in the lab?
Joshua – Pluripotency is a function based on the cells’ functions. We don’t really know what pluripotency is. My lab is working on the issue of pluripotency versus totipotency. We know that some embryonic cells will originate all sorts of cells. The problem is that we don’t know which cells have this property until we conduct an experiment. We now have ECT markers; nonetheless, we can’t be sure that the cells we get are ESCs.
Is the ECT population heterogeneous?
Joshua – Something very interesting was discovered recently. You can take a Petri dish with ESCs, choose a cell, test it for pluripotency, and find out that the cell doesn’t do whatever it is that you want it to do. That cell cannot evolve into an embryo. So you clone this cell in vitro and you get a population of heterogeneous cells. You select a cell from this new population and you discover that it can generate embryo strains. The heterogeneous nature of a cell population seems to be an important element to obtain pluripotent ESCs. A single cell doesn’t perpetuate pluripotency. This is obtained through a complex mix of cells. The interesting aspect about mammals is that if you have a population of embryonic cells in their very early stage, and you cut these cells in half, the result will be two normal embryos. Cells are very regulating. They can regenerate the cells they need next to them in the embryo; they can regenerate this niche. In a sense, we conduct an evolutionary mini experiment when we select a cell that can generate a strain of embryonic cells.
Jennifer – We have discussed this issue with people who work with pluripotency. These people say that the ESCs have to be homogeneous; they all have to be in the same condition. The ideal situation would be for all the cells of the ETC population to be pluripotent and that any cell could be worked on. But we don’t agree with this view.
Joshua – The prevailing mentality is that there is a recipe to create identical ESCs that could then be transformed into all the bodily tissues. There are multiple – and not only a single – types of ESCs. Researchers who study the nature of ESCs already know this, but many people, for example, the people who are trying to use ESCs to produce beta cells in the pancreas to make insulin, do not.
Jennifer – The ESCs are the mammals’ development model. In our opinion, evolutionary biologists understand ESCs better than anybody else does. Unless you understand how an embryo develops, you will not be able to reason correctly.
 eduardo cesar
eduardo cesarJoshua Brickmaneduardo cesar
Many of the experiments with ESCs use mouse or rat cells. Why is it more difficult to work with human ESCs?
Jennifer – Because their embryology is different. Human cells are at a more advanced stage of development than those of mice, and this is why we are unable to explore their potential. Let’s go back to the issue of development. When the first human ESCs were obtained in a laboratory, researchers noticed that they needed special conditions. In fact, these cells were more difficult to cultivate than mouse cells. The human tissue is different. The expression of the markers is different. Nowadays we know that human ESCs are closer to the so-called epiblast stem cells (the cells that generate the skin and the nerve tissues] resulting from the embryo that was implanted in the mice. Human ESCs are at a stage referred to as primed pluripotency (not distinct, but directed towards this process) while mouse ESCs are at the naïve (more immature) pluripotency stage.
Joshua – I believe it is a question of time until we have human ESCs that will enable us to work the same way we work with mice.
Jennifer – A lot of work is being done. In the case of human ESCs, we might never be able to get them to the same stage of the mouse ESCs.
Joshua – We don’t know if this is possible. We still need to conduct experiments. Attempts have been made to do this with limited success.
Should research studies concentrate more on human ESCs and less on mouse ESCs?
Jennifer – If we hadn’t conducted studies on animal cells, we wouldn’t have known where to begin our work with human cells. We wouldn’t have known that it would be possible to obtain all these strains in a culture medium.
Joshua – We have to have cells – such as mouse cells – that can be manipulated to do real genetic work. Mouse cells can undergo specific genetic alterations and generate cell strains, from which we can obtain multiple generations with these genetic alterations. These experiments are crucial. We can modify a mouse cell. You can transform mouse ESCs into epiblast cells, which are much closer to human ESCs. This approach can be very productive. But you can’t manipulate human ESCs this way. We have to work with human ESCs and mouse ESCs. We don’t know where innovation will come from.
Do you believe that the press and scientists create exaggerated expectations about the therapeutical possibilities of ESCs, similar to the exaggerated expectations that were created by the human genome sequencing issue?
Joshua – We need to make a distinction. Therapies based on stem-cell transplants (adult stem cells, extracted from bone marrow) have existed for 30 years. But I agree that expectations have been exaggerated. Scientists must promote realistic expectations about their research. But many scientists are more concerned about attracting the attention of the press or about getting funding for their projects based on promises. The United Kingdom has a funding line at the Medical Research Council that initially encouraged clinical tests being conducted five years after the basic research had been done. This is unreal and holds true in other fields as well. But there is hope in some places. Peter Coffey, from Great Britain, is using ESCs to treat macular degeneration. This is very exciting. But are we going to cure Parkinson’s or muscular dystrophy tomorrow? Of course not. We have to be realistic. These are long-term – 20 or 30 years – objectives. And it might happen that all the research work being done on ESCs might not lead to any cell therapy. But maybe we will be able to identify factors that the cells produce and that could be used to stimulate the body’s endogenous repair, which is much more exciting. I think we will use ESCs in fields that already have protocols that use adult stem cells, such as leukemia or type 1 diabetes [transplants of cells from cadavers’ pancreas]. This is not going to happen tomorrow. It might happen 5 or 10 years from now. We´re not going to cure all diseases with ESCs.
 eduardo cesar
eduardo cesarJennifer Nicholseduardo cesar
What about the research on induced pluripotency stem cells (iPS)?
Joshua – Five or six years ago, many people switched from research on ESCs to research on iPS. Nowadays, I see that they are asking the same questions as I am. They merely changed their study model. The iPS are not the same as the ESCs. Many changes are made to adult cells to turn them into iPS, to make them regress to that stage. There is a higher chance that tumors will be generated when distinct cells stemming from iPs are placed in animal models. We must keep in mind that cancer is a transformation and the iPS are genetically modified cells. The ESCs may have a similar phenotype to that of cancer, but they are genetically normal. An iPS cell is no longer genetically normal; it has been modified. I would be afraid of injecting embryonic stem cells into my body and I would be even more afraid of using iPS, about which many questions still need to be answered. This is why it’s important not to stop researching ESCs just because iPS cells are available.
Jennifer – Let’s go back to the issue of how to differentiate human ESCs. The iPS are not as good as we would like them to be. But I think they are a fantastic line of research.
Why would you like to open a permanent base for the course on ESCs in Brazil?
Joshua – Jennifer and I attended this course, based on the course designed at Cold Spring Harbor [in the United States], which has been held in different places in the last seven years. Now we would like to set up a permanent base, which would make it easier to manage the program. We need investments and a structure to bring researchers from abroad. São Paulo has the resources, the facilities, and the people to do this. The course can only be held where research exists, as this is a two-way relationship. Research helps the course and the course helps the research. There aren’t very many places of this kind.
Jennifer – People are afraid that if they set up a structure for the course and things go wrong that they won’t be able to deal with the situation. But I always say: yes, things can go wrong. But you can fix them. Things are not that complicated. The two us will visit the program at least every two years; in addition, we will bring other people in. And we can be contacted any time by the students.
Joshua – We had a meeting with Professor Mayana Zats’ students from the University of São Paulo’s Center for Studies on the Human Genome. Their enthusiasm is impressive. One doesn’t see this kind of enthusiasm in Europe. We must not forget that not only Brazilian students but also students from Latin America and Europe will attend the course. These students will create an international collaboration network; they will visit each other and they will become department heads at universities some years later. We are going to train young professors and students enrolled in doctoral programs.
What do you teach in the course? How to differentiate ESCs?
Jennifer – This is just a small portion of the course. The most important thing is for students to establish connections, to know what can be done. Of course, we are going to teach practical aspects as well. Their work will not be perfect, something will always go wrong, but they will be able to count on their course-related contacts to solve problems. We like to believe that we teach students to think critically. They are the target of mine and Joshua’s bullying.