In a matter of three months—from December 2019 to April this year–the novel coronavirus from China infected 926,000 people in 180 countries, causing a respiratory disease that is similar to, but more serious and lethal than, the flu. In that short space of time, 46,000 people died (including 240 confirmed deaths in Brazil as of April 1). An initial analysis of data for Brazil, compiled by researchers at São Paulo State University (UNESP), the University of São Paulo (USP) and the Federal University of ABC (UFABC), indicated that in this early phase of the pandemic the number of cases doubled in the country every 2.5 days. As the coronavirus pandemic—possibly the fastest-spreading pandemic in the last 100 years—grew to global proportions, the public was barraged with information in real time, often describing concepts laypeople were not familiar with. One concept that has dominated the news media is the epidemic curve, along with the notion that the curve has to be flattened to prevent healthcare systems from being overwhelmed.
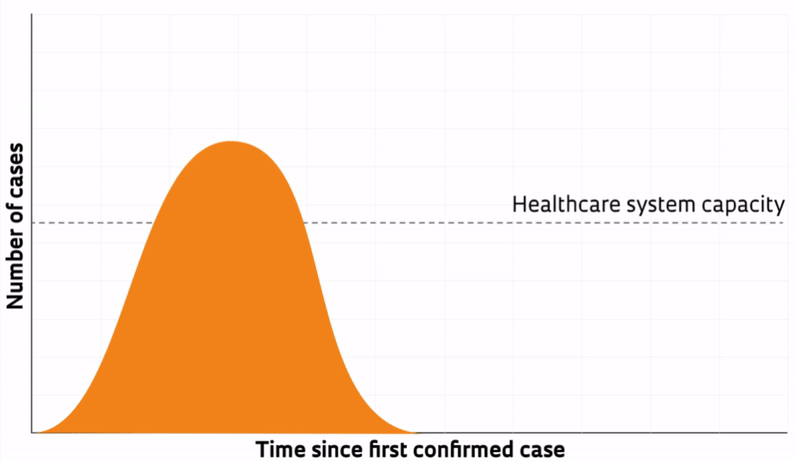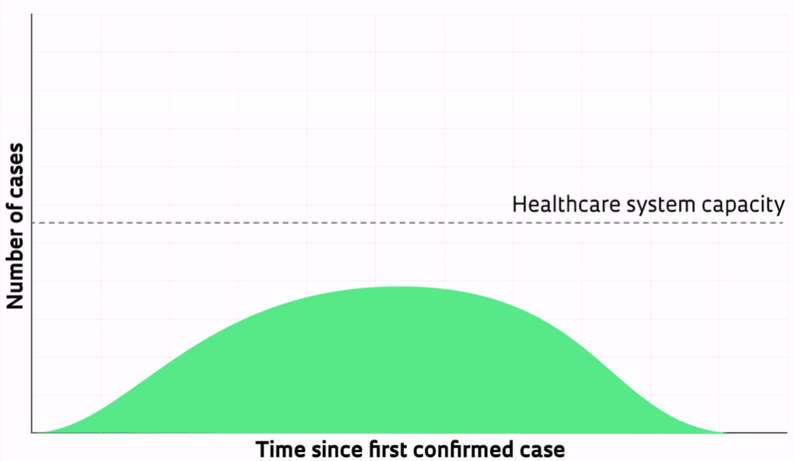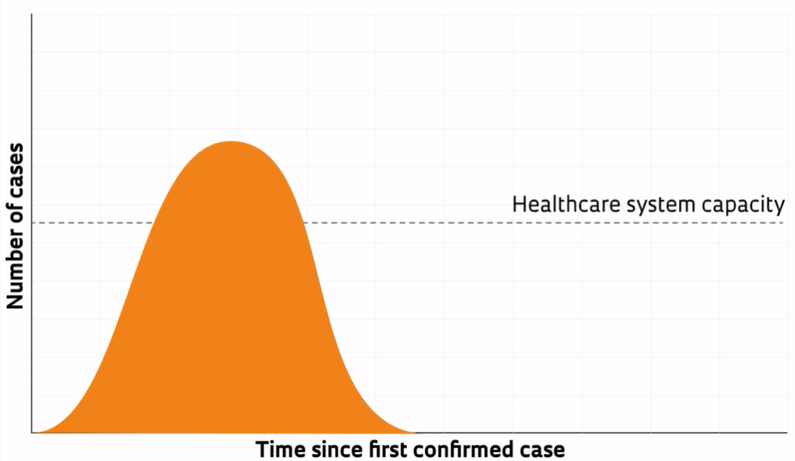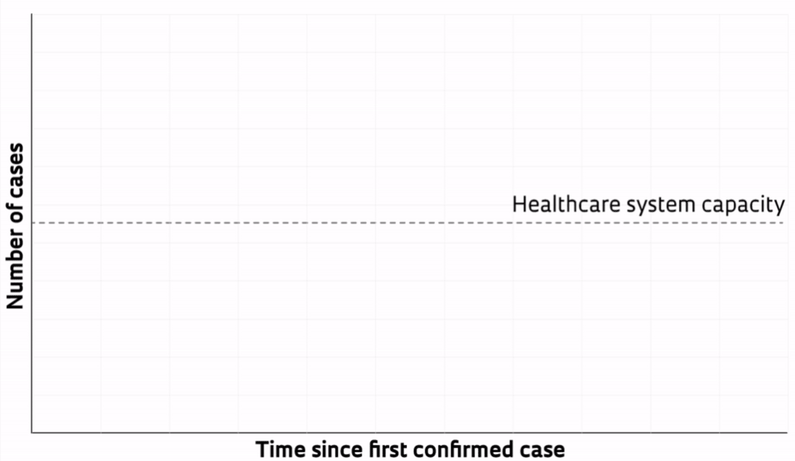
But what does it mean to flatten the curve? An epidemic curve is represented by a simple graph that is useful for health authorities. One of the basic tools in the epidemiologist’s toolbox, an epidemic curve shows the number of cases over time and the initial evolution of a disease, helping to plan the public-health response. Many new diseases that have plagued humanity over the years have exhibited similar behavior and typically resulted in a characteristic, bell-shaped epidemic curve. After being featured in The Economist in early March, the graph became popular in global news media as a simple way of depicting the challenge that healthcare systems around the world are facing in containing the spread of Sars-CoV-2, the novel coronavirus that causes COVID-19.
Like the epidemic curves for other infections, the new coronavirus curve has been divided into three vertical sections—a left, a middle, and a right section—to analyze the progression of the disease. The left-most section is the one that currently has health authorities’ attention. For new infections with the potential to spread across the entire population, this part of the curve describes the phase of exponential (accelerated) growth. In this phase, the number of cases rises at such a fast rate that the total case count nearly doubles within a few days. The higher the pace of growth, the steeper the curve.
Epidemiologists and health authorities focus on this part of the curve because it describes the rate of progression of the disease and predicts when the epidemic will reach its peak. If initial growth rates are too steep, the number of cases can quickly overwhelm and cause healthcare systems to collapse, as occurred in February and March in northern Italy.
“From a public-health perspective, this initial phase is the time to act—and quick—to slow the spread of the epidemic and reduce the height of the peak as much as possible,” says physicist Roberto Kraenkel of the UNESP Institute of Theoretical Physics, who works with mathematical models in the fields of ecology and epidemiology. In a collaboration with researchers from USP and UFABC, Kraenkel created the Covid-19BR observatory, which uses data from the Brazilian Ministry of Health to monitor the evolution of the coronavirus pandemic in Brazil. Based on available data as of March 17, when there were 291 confirmed cases in Brazil, the group calculated one of the parameters affecting the acceleration phase of the epidemic: the time it takes to double the total number of cases, which in mid-March was 2.5 days.
Slowing the initial rate of spread and consequently flattening the curve is essential in preventing hospitals and intensive care units (ICUs) from being overrun. Only 20% of people infected with Sars-CoV-2 show symptoms, according to estimates. Of these, 14% require hospitalization and 5% end up in the ICU. Because bed numbers are limited, a rapid increase in infections and serious cases can quickly exceed the country’s hospitalization capacity—Brazil has approximately 450,000 public and private hospital beds, of which 41,000 are ICU beds, according to a 2016 survey by the Brazilian Association of Intensive Care Medicine. If infection rates are successfully reduced, the peak of the epidemic is spread out over time, and fewer people require hospitalization simultaneously. This results in fewer infections and fewer deaths, as explained by Anthony Fauci, director of the US National Institute of Allergy and Infectious Diseases, during a press conference on March 10.
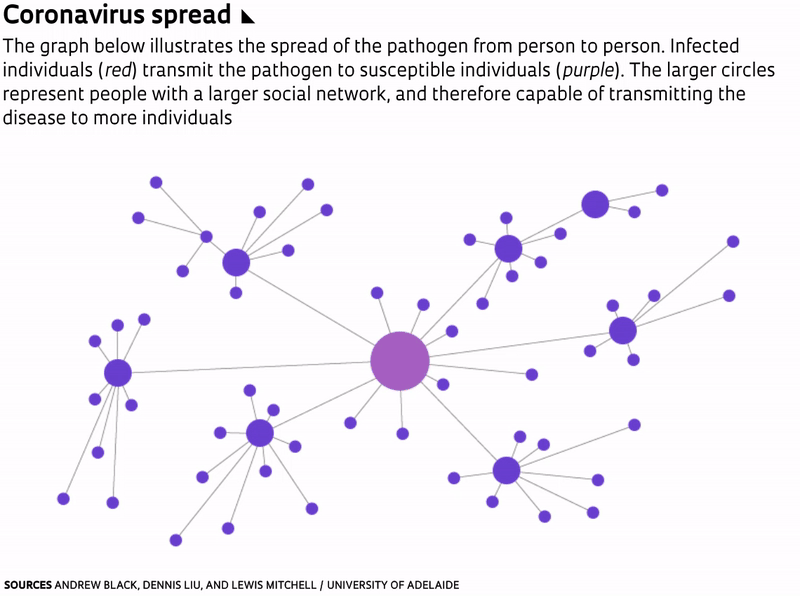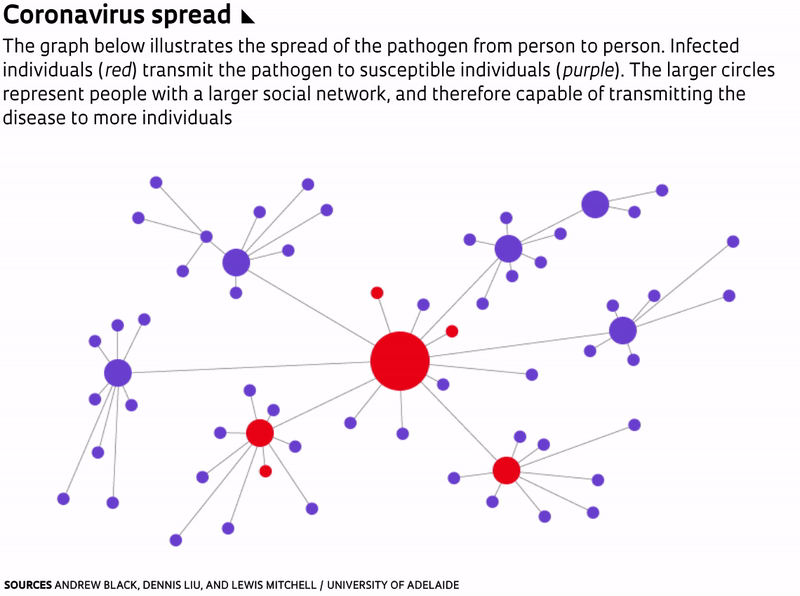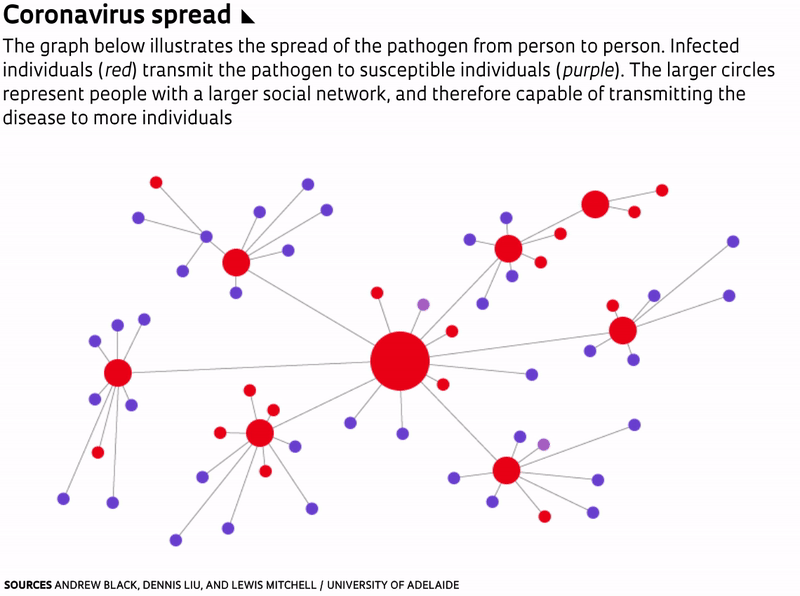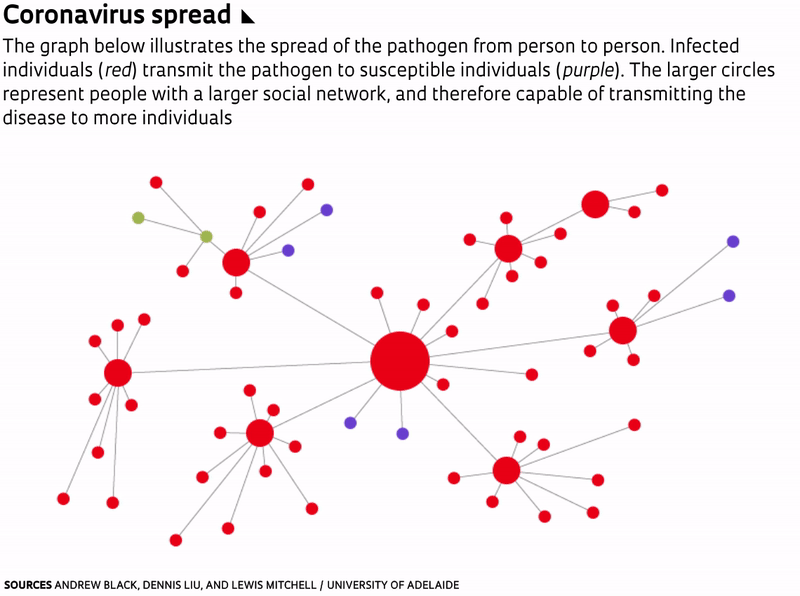
One of the ways to flatten epidemic curves is through vaccination. But because a vaccine for the novel coronavirus has yet to be developed and tested, the most effective measures now available are social distancing and sheltering in place. This reduces the number of people to whom an infected individual can transmit the virus. “In doing so, the same number of people will probably be infected, and the epidemic will last longer, but the number of severe cases will be spread out,” wrote mathematicians Andrew Black, Dennis Liu, and Lewis Mitchell of the University of Adelaide, in Australia, in a paper published on March 16 in The Conversation.
But apparently the explosive nature of the initial phase can be used to advantage in accelerating containment. This would require, however, that the initial response begin as early as possible, explains British epidemiologist Britta Jewell, a researcher at Imperial College London and an expert in infectious disease modeling, in an interview published on March 11 in The New York Times. Using US coronavirus data as of mid-March, when the number of cases was rising by 30% per day, she projected what would happen if steps such as canceling events and restricting travel were taken now rather than one week from now. “If you act today, you will have averted four times as many infections in the next month: roughly 2,400 averted infections, versus just 600 if you wait one week,” says the researcher.
Republish